Report Published March 30, 2015 · Updated March 30, 2015 · 19 minute read
Make Health Care More Convenient and Coordinated with Medical Homes

Lower back pain can feel like sharp stabs radiating from your spine. When back pain struck a 45-year-old Marylander on a Saturday in 2014, his first thought was to go to the ER, but then he remembered to call the nursing staff hired by his health plan to triage his health care needs.1 A nurse referred him to a doctor’s office with weekend hours where the doctor diagnosed muscle spasms and advised heat applications and over-the-counter ibuprofen. By Monday, he felt good enough to cancel a follow-up appointment and go to work. He avoided missing work and a hospital bill that would have cost thousands of dollars. And the doctor’s office helping him shared the savings from the prevented ER visit. Under this program, CareFirst Blue Cross Blue Shield patients have had 6% fewer hospital admissions, 8% fewer readmissions, 11% fewer days in the hospital, and 11% fewer outpatient visits than other CareFirst members.2
This medical home model provides patient-centered, coordinated care with a focus on the needs of each person. It works around their lives rather than making them follow a doctor’s schedule. Adopted nationally, it would also save money—trimming $148 billion from the federal budget over ten years due to less waste and more effective care.3
This idea brief is one of a series of Third Way proposals that cuts waste in health care by removing obstacles to quality patient care. This approach directly improves the patient experience—when patients stay healthy, or get better quicker, they need less care. Our proposals come from innovative ideas pioneered by health care professionals and organizations, and show how to scale successful pilots from red and blue states. Together, they make cutting waste a policy agenda instead of a mere slogan.
What Is Stopping Patients From Getting Quality Care?
Problems that are simple to treat in a physician’s office can spiral out of control without proper care and assistance for patients. Patients with diabetes can end up blind or have a foot amputated without routine care and support. Patients with asthma can end up in the ER unless they have, and know how to use, medications that prevent asthma attacks. Patients who leave the hospital and don’t receive prompt follow-up may mix up new medications or miss warning signs, leading to another, and unnecessary, hospital visit. All of these examples are bad for patients and costly to taxpayers.
Often, patients only need quick access to health care through a phone call or email that does not involve a multi-hour trip to see a physician. They also need health care that does not wait for something to go wrong when a standard check-in would prevent it. Just as today’s cars have built-in reminders for preventive maintenance, there is no reason that health care professionals shouldn’t be flashing signals to patients that it is time to check in.
But today, physicians do not receive payment for care when answering patients’ phone calls, responding to emails, or sending care alerts. The traditional form of payment comes from seeing a patient in the office or performing a procedure. It is shocking that in the modern era of instant communications, physicians have little incentive to use them. Even though gaps in care can be harmful and lead to additional care by specialists, making sure they don’t occur has no monetary value to primary care physicians under traditional payment systems.
The lack of attention to basic care adds up to unnecessary costs and suffering. This is especially true with patients who have multiple chronic conditions. If they do not receive help managing those conditions, their health can spiral out of control and land them in the emergency room. In fact, nearly 60% of emergency room visits among Medicare patients are potentially preventable.4 Furthermore, the average cost of an emergency room visit for Medicare patients increased from $720 in 2000 to $1,062 in 2010, a 47.5% increase.5
Where Are Innovations Happening?
Innovative efforts that coordinate care have sprung up all across the country because of a desire to help patients manage their chronic conditions and get the best care. These efforts—called medical homes—can and do help patients requiring many different types of care. The Patient-Centered Primary Care Collaborative (PCPCC) houses a comprehensive list of these innovations and represents over 1,200 medical home efforts in the U.S.6
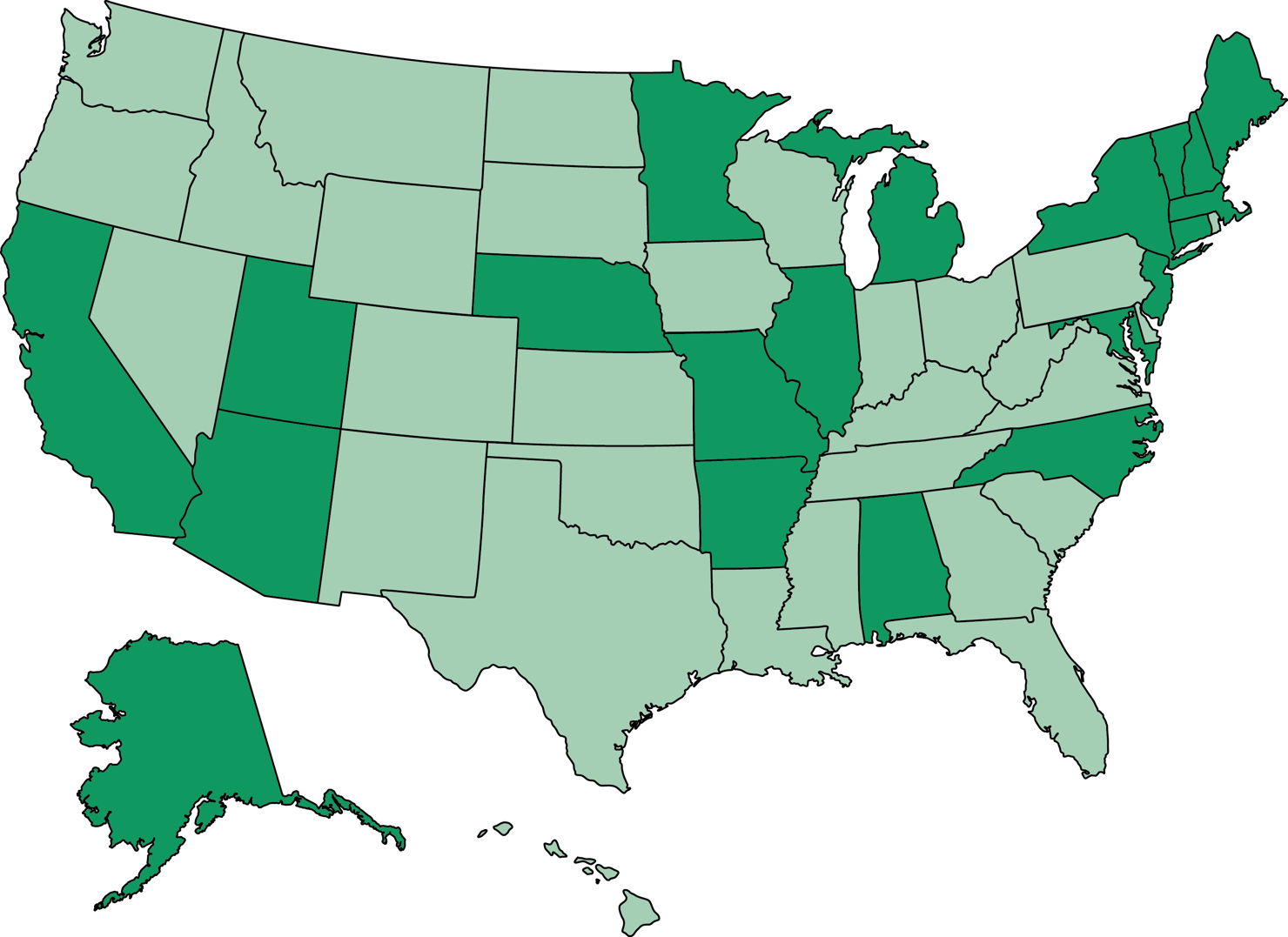
Every state has a medical home initiative. Initiatives in the darker shaded states are highlighted in the local examples memo.
Instead of only seeing you when you’re sick, medical homes focus on keeping you healthy and supporting you if you have a chronic condition. Think of it like a cocoon. It is a warm and supportive team of health professionals, led by a physician, who watches over your health using modern communications and information technology. This may mean reminder calls from a nurse, a nutritional expert on staff, or support groups for those facing similar medical challenges, such as diet changes for those with diabetes.7 These enhanced primary care offices also take the extra time to communicate with the other providers you may see, like specialists, hospitals, or home health aides, so that your care is coordinated and you avoid duplicated tests or conflicting advice. Most importantly, health care providers offering medical homes are accessible—keeping longer hours and communicating over the phone and via email.
Doctors and other health professionals who run medical homes anticipate their patient’s needs and arrange for the right resources to address those needs. They use an electronic health record system to see and plan for the full range of problems their patients’ are at risk of developing or already have. For example, if patients are having trouble taking their medications, a pharmacist who works with the medical home team may help patients manage their medications. A medical home practice may include a variety of health professionals who provide and coordinate care like nurse practitioners, nurse, social workers, and medical assistants, a rapidly growing health care profession.8 Also, smaller practices often work with other organizations like a health plan to organize the needed staff.
A medical home practice also provides access to care beyond normal business hours as well as alternative means of communicating with its staff rather than an office visit—such as through phone, email, and video conferencing. Such communication also includes planning a patient’s visit to the office when it is necessary as well as follow-up after the visit. Indeed, patients with a variety of cultural, ethnic, and racial backgrounds all need to feel confident about how to engage the practice, that there’s a plan in place for the care they need, and how to handle problems not anticipated in the plan.
These many types of functions are formally recognized in certification programs for patient-centered medical homes. For example, the National Committee for Quality Assurance lets medical homes seek and receive recognition that, in some instances, health plans can use as a basis for paying the enhanced primary care services.9 Such services can also include behavioral and oral health care. Regardless of a formal recognition program, health plans can assess the overall impact of medical homes based on objective data about patients’ health outcomes, experience and cost of care.
Health plans in a number of states, including those offering Medicare Advantage, have successfully experimented with new ways to pay for this type of enhanced primary care using the savings from preventing emergency care and other avoidable procedures. For example, Anthem operating in Colorado, New Hampshire, New York, and elsewhere offers monthly lump sum payments to physicians that cover email and telephone communication with patients and coordination of a patient’s care with multiple physicians.10 The health plan then tracks how well the physicians’ patients do against 35 measures of success. If the patients maintain good health at lower costs, then the physicians share in the reward, as much as 30% of the savings.
In addition to payment of a care coordination fee, another strategy to support medical homes comes from CareFirst in Maryland. It assigns a nurse to each physician to support the extra time needed to communicate with patients and coordinate their care.11 That has helped get the program up and running with physicians who don’t have the time or resources to hire additional staff. Such pilot programs have lowered ER visits by 37%.
A third strategy has been put to the test in Indianapolis by Wishard Health Services, which is affiliated with the Indiana University School of Medicine. The GRACE program (for Geriatric Resources for Assessment and Care of Elders) provides a rich set of services including (1) physicians trained in geriatric medicine; (2) in-home assessment and care management provided by a social worker and nurse practitioner team; and (3) coordination of many kinds of care ranging from pharmacy to mental health and from home health to inpatient geriatric care services. It reduced hospitalization rates by 44% among patients who otherwise would have likely been admitted to the hospital.12
In seven regions around the country, 38 different public and private payers are already working together to align their medical home efforts through the Comprehensive Primary Care Initiative launched by Medicare.13
In each market, payers have agreed to common requirements for medical homes, quality measures, and payment methods, as well as the same selection process, so that their investments are targeted at the same transformation-ready practices. This collaboration was only possible because Medicare was willing to play a central convening role—allowing private payers to discuss operational alignment without traditional anti-trust violation concerns. So far, 2,437 providers at nearly 500 sites are receiving these payments and are accountable for rigorous quality and cost-savings milestones.14
How Can We Bring Solutions To Scale?
As a result of these successful state initiatives—and many others—medical homes should be scaled and implemented nationwide. Medical homes need not be limited to the traditional fields of primary care, namely family medicine, internal medicine, and pediatrics. Certain patients, for example those with mental health problems or those newly diagnosed with cancer, would benefit from the enhanced communication and care coordination available through specialists who offer medical homes.15 Other health professionals, such as pharmacists and nurse practitioners, also have key roles to play in successful medical homes. They often have the time and specialized skills to support patients in a holistic way, following through on drug regimens and managing chronic diseases.
To successfully increase the adoption of the medical home model, policymakers should take the following two steps:
1. Medicare, Medicaid, and all other federal health programs should offer medical homes to beneficiaries through their physicians.
The expansion of medical homes through federal policy should build up from the foundation laid by the Centers for Medicaid and Medicaid Services (CMS). The CMS Comprehensive Primary Care Initiative has worked with multiple stakeholders to develop support for enhanced primary care across five critical functions: (1) care management based on the risk profile of patients; (2) access and continuity of care; (3) care plans for patients with chronic conditions and for preventive care; (4) patient and caregiver engagement; and (5) coordination of care across all health care providers, also known as the medical neighborhood.16
The key step to a national implementation of medical homes is a new payment method through federal programs for the bulk of primary care. Specifically, it would boost payments to primary care professionals in three possible ways:
- It would provide a lump sum payment for services that cover modern communications and care coordination, which would most often be a monthly payment for each patient.
- Primary care physicians could receive additional payment bonuses by sharing in savings that occur when their patients do not end up going to the ER or the hospital for preventable problems.17
- Primary care physicians could also receive a comprehensive payment for all of their patients’ health needs. Such payment changes can also include rewards for health professionals who increased the quality of care for their patients instead of paying them more for performing potentially unnecessary tests.
The implementation of medical homes would vary by the insurer or provider organization. In original, fee-for-service Medicare, for example, physicians would have two choices about how to participate. They could: (1) implement the medical home model and receive incentives directly; or (2) use an administrator, such as a physician organization, that would handle the management of costs and payments under a contract with Medicare. Initially, physicians would have the opportunity to receive incentives if they choose to participate, but after five years, physicians in primary care fields that do not adopt the medical home model would face penalties in the form of declining reimbursements.18
2. Medicare should partner with states and private insurers to accelerate the adoption of medical homes for all patients and payers.
As essential as these changes are, Medicare patients represent only a portion of any primary care practice. To truly change the delivery of care, and to maximize the associated savings, public and private payers will have to work together.
Like all of us, doctors are creatures of habit, and the changes necessary for a medical home to succeed—new forms of communication and providing care coordination through a team-based model—don’t just require new resources, they also require changing a physician’s daily routines. Behavioral science has demonstrated that incentives can be effective at changing behavior, but only if they are well-designed and consistently aligned with the end goals. If physicians are only incentivized to provide online communication or team-based care coordination for Medicare beneficiaries, then it will be challenging to transition their entire practice into a medical home because they may be incentivized to do the opposite for patients with a different insurance. With different incentives at odds, physicians are less likely to change their behaviors. In order to best align incentives for a physician’s office to transform into a medical home, it needs to transform for all patients—and this means private payers need to be involved too.
Medicare has several promising demonstrations underway to expand the scope of medical homes, including innovative multi-payer efforts like the Comprehensive Primary Care Initiative.19 This means private insurers, major employers, and state Medicaid programs partner with the federal government to pay physicians in the same way for acting as medical homes. Multi-payer efforts not only support total transformation of physician practices, they also share the cost of implementing medical homes—maximizing Medicare’s return on its investment—and reduce burdens on providers because there are common participation and quality reporting requirements.
Congress should authorize this expansion in anticipation of success with the demonstrations and make participation in aligned private payer initiatives a condition of receiving medical home funding from Medicare. Such a requirement for providers will build demand in the marketplace for payers to not only offer patient-centered medical home payments, but also to use a common model for their programs. To ensure that payers use a common model, Congress should direct Medicare to either lead multi-payer collaborations or participate in them in each area of the country. Congress should also give Medicare fiscal flexibility to provide upfront funding for medical homes, regulatory flexibility to reduce barriers to medical homes, and anti-trust relief to allow payers and providers to collaborate with each other and the federal government. Congress should also ensure that federal and state rules enable the development of online health care, which is also known as tele-health.20
Potential Savings?
According to an analysis by the Actuarial Research Corporation, providing medical homes to high-risk patients would save the federal government $147.6 billion over ten years and the whole health care system a total of $229.8 billion over ten years.21 The chart below shows the year-by-year savings for each program.
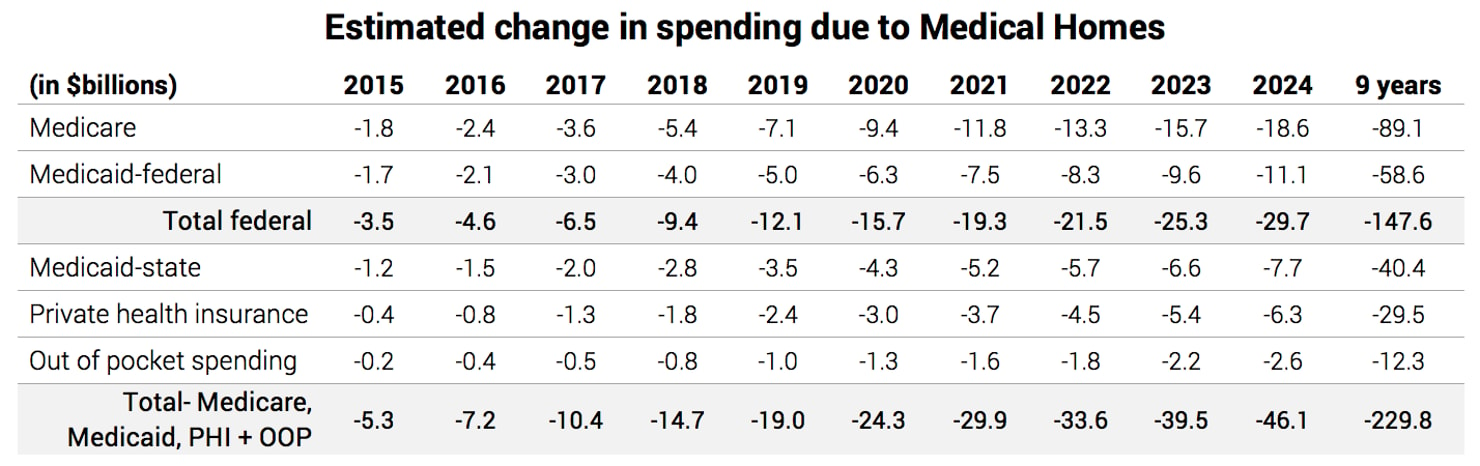
Questions & Responses
Are medical homes voluntary for patients?
Yes, patients would be free to choose whether or not to use the services offered under a medical home. As more doctors adopt the medical home model, they would likely become the norm for most patients.
Do medical homes reduce patients’ access to specialists?
No, a patient-centered medical home is not meant to reduce access to care. Instead it is a pro-active, team-based model that is meant to provide coordinated, timely, and efficient access to the most appropriate care.
Because of the enhanced care that medical homes provide, they may prevent unnecessary specialty care that the patient may have otherwise required. For example, by helping patients with diabetes control their disease, a medical home keeps patients from needing specialized care for a failed kidney that diabetes could have caused. It also helps make sure patients with diabetes get access to specialists like an ophthalmologist who can prevent and treat blindness that diabetes can also cause when left untreated. When a patient needs specialized care, a physician providing a medical home will help coordinate the care.
Do patients need to switch physicians to have a medical home?
Any physician who leads a patient’s care would be able to offer a medical home. Typically this means a patient’s primary care provider, but for some patients with specific needs, a specialist may fill this role. These physicians would receive reimbursements for the upfront cost of additional services provided under a medical home and for identifying patients with the greatest needs. Although it would take several years for all medical practices to develop the capacity to offer a medical home to their patients, all primary care physicians would have a strong incentive to do so eventually.
Do physicians have to join a big group practice to offer a medical home?
No, both small and large medical practices can offer medical homes. While larger groups may have some economies of scale in terms of lower fixed costs for big ticket items (e.g., electronic medical records), smaller practices can be supported with such infrastructure arranged through a health plan or community-based resources.
Will medical home services be available to all patients or only those with the most complex medical needs?
Under Third Way’s proposal, physician offices would be expected to serve as medical homes for all of their patients—not only the sickest. Though some studies highlight that medical homes are most cost effective for patients with multiple chronic conditions, behavioral economics teaches us that aligning incentives for physicians to provide care is mostly likely to lead to doctors as quarterbacks for care coordination. In order to see the largest benefit for the sickest, we must also invest in total practice transformation that includes those who need only preventive services. To reduce the costs of including all patients, medical home payments could be tiered according to the severity of patients’ medical needs, with practices receiving smaller payments for patients who require less care coordination.
What about medical homes run by nurse practitioners?
In many states, nurse practitioners, who have advanced training, can practice independently from physicians. All payers including Medicare should allow them to run medical homes where those states allow them such independent practice. This step would expand patient’s access to medical homes in rural America and other areas with little or no access to physicians.22
What can be done to ensure full participation of pharmacists in medical home practices?
Pharmacists are currently at a disadvantage when participating in new shared savings programs used to advance medical homes and other new payment models under Medicare because payments for their medication management services do not come through Medicare directly as they do for all other allied health care professionals. Congress should authorize direct payments to pharmacists for medication management services by pharmacists participating in new payment models such as medical homes. That way pharmacists would be on an equal footing as other health professionals in the distribution of shared savings.
Is Medicare’s recent decision to pay for care coordination sufficient to create a medical home?
No, but it is important progress. In December of 2013, CMS announced that Medicare would begin covering care coordination for chronically ill patients starting in January 2015. Approximately two-thirds of Medicare beneficiaries have chronic conditions, so this is a large step in the right direction.23
Is telehealth an effective way to give patients more access to medical homes?
Yes, but state laws sometimes limit or prohibit online health care visits with physicians. The medical home model can utilize telehealth to improve care coordination to increase communication between patients and providers. However, no two states define or regulate telehealth in the same way.24 Medicaid policies defining and paying for telehealth differ across states. Alignment with Medicare payment policy is also not guaranteed—and private payers do not consistently reimburse for telehealth across states. Often, there are even inconsistencies on telehealth policies within states.25
How will policy-makers and private insurers know which medical home models are working best?
The Patient-Centered Primary Care Collaborative is one the major groups pushing for adoption of medical homes in the public and private sectors.26 Its membership represents more than 1,000 stakeholder organizations and 50 million health care consumers. It has extensive information about medical homes being developed throughout the U.S.
How do medical homes fit with legislation that would reform physician payments in general?
Medical homes are one part of a larger set of reforms to change physician payments under Medicare. For example, several recent bipartisan reform efforts have proposed replacing the current fee-for-service payment system with other payment systems like medical homes, accountable care organizations, or bundled payments.27 After several years of development and refinement of new payment models, physicians would have to choose between being reimbursed through a new payment system or facing penalties in the form of declining payments for fee-for-service reimbursements. As a new Congress takes up the critical question of Medicare payment reform, incentives for providers to create medical homes could be included in a wide range of broader policy designs.
What comes next? Are there longer-term visions for reforming primary care payments even beyond patient centered medical homes?
Patient centered medical home programs, particularly multi-payer initiatives, not only support patient care in the present, they also do the important work of defining what a high-functioning primary care practice looks like, and what services it should perform. Some health policy leaders have called for building on this model to create a new Medicare provider category for advanced primary care practices—separate from the Physician Fee Schedule—that would pay providers who meet certain requirements in a whole new way.28 Such a policy would make the patient-centered medical home type payments the basis for primary care reimbursement, rather than just an add-on to the fee-for-service system.

