Memo Published March 30, 2015 · Updated March 30, 2015 · 20 minute read
Local Examples: Innovations in Patient-Centered Medical Homes

Problems that are simple to treat in a physician’s office can spiral out of control without proper care and assistance for patients, leading to hospital visits that could have been avoided. Individuals also need health care that does not wait for something to go wrong when a standard check-in would have prevented it.
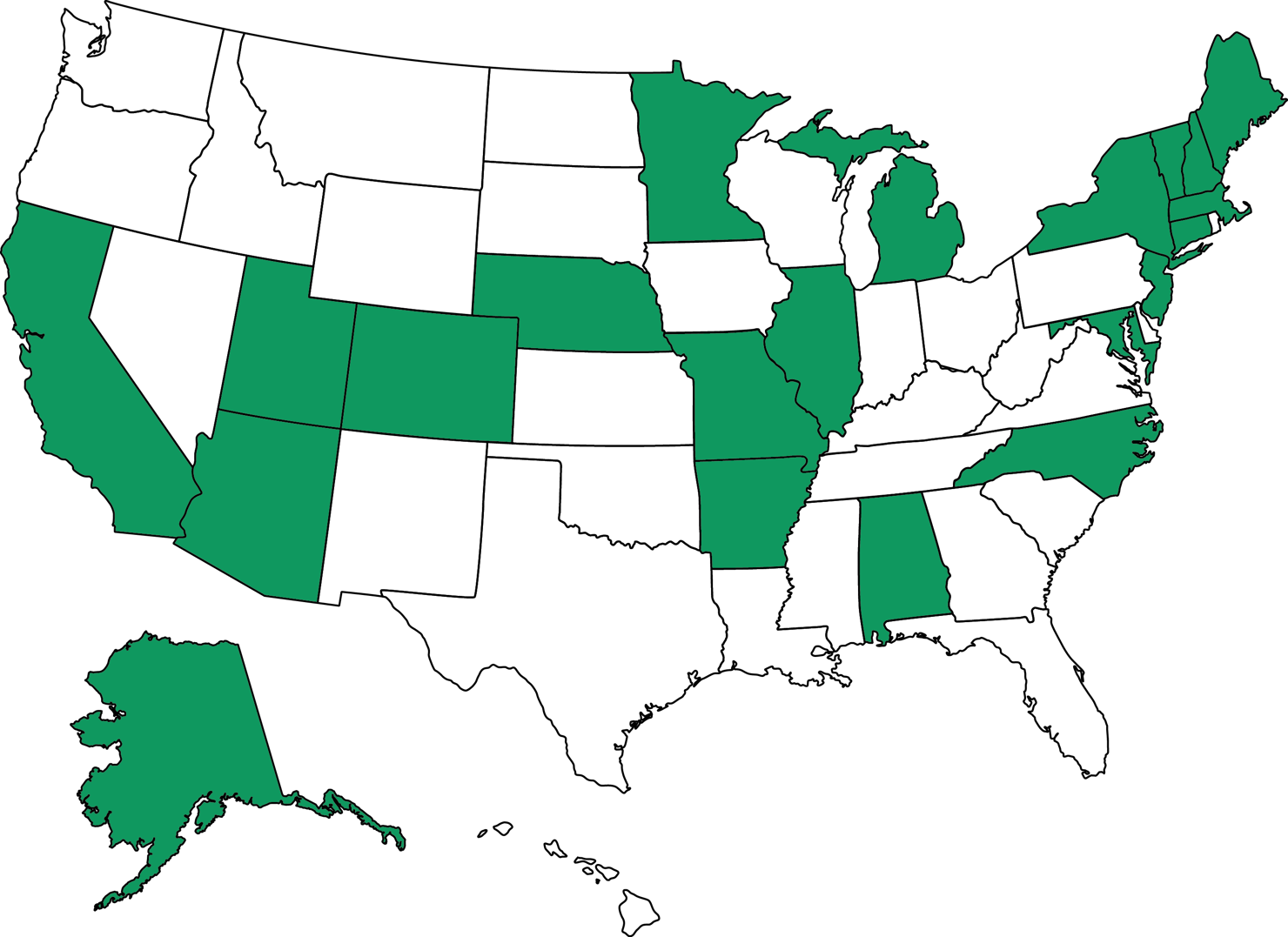
Innovative efforts that coordinate care—called medical homes—focus on keeping patients healthy with a supportive team of health professionals, led by a physician, who watches over your health using modern communications and information technology. Medical homes have sprung up all across the country, with some states or private payors implementing state-wide initiatives, all which improve the quality of care and patient experience while generating real savings from preventing emergency care, hospitalizations, and avoidable procedures. Below are three stories that show how medical homes change the patient experience and several other examples of innovations from all over the nation compiled by the Patient-Centered Primary Care Collaborative.
Blue Cross Blue Shield CareFirst Patient-Centered Medical Home, Maryland and D.C. area:
A 45-year-old resident of Maryland was stricken with severe lower back-pain on a Saturday in 2014. Like many individuals faced with health care needs outside of normal office business hours, he considered heading to the emergency department. There, he would have likely gone to radiology for X-rays or other expensive scans and then had a referral to a specialist. Luckily, this particular patient was covered by CareFirst Blue Cross Blue Shield, which had started a medical home program in Maryland and the DC region. High-risk CareFirst members are assigned nurses from an independent company, called Healthways, that CareFirst pays for—who are available by phone to monitor care and help navigate the system.
Instead of heading to the ER, the patient called to check in with a Healthways nurse, who directed him to the primary-care practice that was open on weekends. The doctor there diagnosed muscle spasms and advised heat applications and over-the-counter ibuprofen. The patient felt good enough to cancel a follow-up appointment and return to work Monday. Not only did he avoid time away from work and a hospital bill that would have been thousands of dollars, but the primary care team serving him also shared in the savings from the prevented ER visit.
CareFirst shares these savings with groups of physicians and nurse practitioners ranging in size from five to 15 primary care providers. Every participating provider also receives increased fees in exchange for the extra effort and time devoted to improved coordination of care and the creation of care plans for their sickest patients. They can share in robust bonus payments for improving quality and reducing costs.
The program has more than paid for itself according to CareFirst and improved the quality of care. In 2013, members participating in the medical home experienced 6% fewer hospital admissions, 8% fewer readmissions, 11% fewer days in the hospital, and 11% fewer outpatient visits than other CareFirst members.
UCLA Mattel Children’s Hospital Pediatric Medical Home, California:
Chronically ill children and their families have to juggle care from as many as nine different specialists when dealing with their conditions. Giselle, a California child born with a rare genetic condition, has had 65 surgeries in her life. She’s dealt with seizures, pituitary problems, blindness, and cataracts. Her health care needs don’t always fall neatly into her specialists’ schedules. If her doctors at UCLA’s Mattel Children’s Hospital hadn’t started their pediatric medical home, she and other patients like her would have had to coordinate their own appointments and make sense of treatment options from multiple specialists—and likely would have resorted to using the emergency room to get needed care.
UCLA’s medical home provides family-centered, coordinated care with a focus on each individual child and a schedule for care that works best for that child and his or her family. The pediatric model includes basic components such as: a formal 60-minute intake appointment, follow-up appointments of 40 minutes, access to a bilingual family liaison to help families navigate the medical system, and a family binder that keeps all a child's medical information in one place.
In addition to better care for pediatric patients and their families, the model reduced emergency room visits by 50%. Further, this model significantly increases patient satisfaction and makes patients like Giselle feel like the medical home is her “second home.”
Capital Health Plan’s Center for Chronic Care, Tallahassee, Florida:
Jim Carraway, a 53-year-old retired state of Florida employee, suffers from Charcot-Marie-Tooth, a rare neurological disorder that causes progressive nerve and muscle degeneration. He also suffered a stroke, had six heart bypass operations, a defibrillator implanted, several surgeries on his feet, and has diabetes. He was exactly the kind of patient for whom the Capital Health Plan in Tallahassee designed the Center for Chronic Care. When the Center was created in 2003, Capital Health Plan identified their sickest patients, those with multiple chronic conditions who didn’t fit into existing programs for patients with single diagnoses, and, after consulting their primary care physicians, invited them to the Center for Chronic Care. Here, using a comprehensive, planned approach to care with a focus on patient engagement and self-management, every aspect of a patient’s care is coordinated. If a patient is admitted to Tallahassee Memorial Hospital, the largest hospital in the area which serves a significant percentage of the area’s residents, or visits the hospital’s ER, the hospital’s electronic health record flags the patient so that the Center for Chronic Care’s medical director can be closely involved in their care. Capital Health Plan has seen primary care physician visits and pharmacy costs increase for the Center’s patients, but inpatient hospital days dropped by 40%, ER visits decreased by 37%, and overall claims costs for these patients dropped by 18%. The care model makes a difference for patients like Jim Carraway who, according to his wife, Sarah, is “doing much better” than he was before becoming a patient of the Center. Jim says that at the end of each visit, his doctor sets “goals and expected outcomes for the next visit, like lose five pounds or keep your blood pressure at this level. He names them, and it is motivating, because you know someone is paying attention.”
Alabama
- BlueCross BlueShield of Alabama Primary Care Value Based Payment Program: After the completion of a successful medical home pilot program which resulted in fewer emergency room visits, fewer hospital days, increased patient satisfaction, increased use of preventative services and yielded over $1.9 million in cost savings, BCBS Alabama launched the Value Based Payment (VBP) Program in 2011. The program serves Montgomery, AL, and surrounding areas and targets primary care specialties such as Geriatrics, Family Practice, and Pediatric Medicine. Primary care physicians earn points in three performance measure categories toward a maximum reward potential of 20% of all billed medical and surgical codes.
Alaska
- Alaska Southcentral Foundation—Nuka System of Care: The Southcentral Foundation is an Alaska Native-owned primary health care system and, in 1999, began the Nuka System of Care focused on physical, mental, emotional, and spiritual wellness, which included components of a patient-centered medical home. Patients are matched to integrated, comprehensive care teams that provide enhanced access to care and improve care coordination. These efforts resulted in lower emergency department use for all causes and, in particular, for visits related to adult asthma. In addition, access to same-day appointments, enhanced office hours, and electronic visits with providers increased, as did preventive services for people with asthma.
Arizona
- Cigna Accountable Care Program—Cigna Medical Group: In 2010, Cigna HealthCare launched the first patient-centered medical home in the Phoenix area consisting of a large medical group practice treating members of a single private payer. With the aim of improving quality and lowering costs, the Cigna Medical Group physician practice focuses on intensive care coordination, particularly for patients with chronic illnesses and ongoing health care needs. Providers that meet quality and cost targets receive financial rewards, and the program has produced in an 11% decrease in outpatient surgery and costs, 7% lower total medical costs, and average annual per patient savings of $336. Overall preventive care visits increased by 3% and adult preventive care visits, in particular, were up 12%.
Arkansas
- Arkansas is putting the full weight of its health care policy-making behind patient-centered medical homes. The Health Care Independence Act, a 2013 state law, requires all qualified health plans sold in the state in the Affordable Care Act marketplace to participate in the Payment Improvement Initiative, which requires plans to designate a “principal accountable provider” for each beneficiary (based on claims data), support patient-centered medical homes, and provide clinicians with performance data. In addition, nearly 80% of the state’s Medicaid beneficiaries have their care coordinated by a patient-centered medical home. A number of statewide multi-payer efforts to advance patient-centered medical homes are also underway, including a $42 million grant from the Centers for Medicare & Medicaid Services (CMS) to test a model for a sustainable, patient-centered health care system.
California
- Brown & Toland Physicians, a large physician network in the San Francisco Bay area created the first National Committee for Quality Assurance-designated Level-3 Patient-Centered Medical Home called My Health Medical Group, and was named the 2013 Patient-Centered Medical Home practice of the year by the California Association of Family Physicians. Brown & Toland extended this patient care philosophy to Medicare beneficiaries as a Pioneer Accountable Care Organization (ACO), providing patients with coordinated care, post-hospitalization assistance, chronic disease education, and health coaches and advocates, among other enhanced services. In its first year as a Pioneer ACO, Brown & Toland saved Medicare $10.6 million and, in 2013, saved Medicare an additional $4.5 million and was one of just 11 Pioneer ACOs to earn shared savings.
Colorado
- As an early adopter of the medical home model, in 2007 Colorado required its Department of Public Health and Environment to increase the number of children served by health homes. The state’s first multi-payer medical home pilot launched in 2009, and in 2011, the state’s Medicaid program created the Accountable Care Collaborative. Under this collaborative, primary care medical providers contract with regional care collaborative organizations to provide medical home services to adults and children enrolled in Medicaid. The goal is to link every Medicaid enrollee with a primary care provider who not only ensures timely access to primary care, but also helps patients access wraparound services such as housing assistance, behavioral health care, child care, and more. This additional support may be provided by the primary care provider directly or through other providers coordinated by the regional collaborative, which helps to coordinate patient care and assists with care transitions. The primary providers and regional collaboratives receive a per-member per-month payment for medical home services and incentive payments for meeting specific performance goals. This program has impressive performance results, including a 15-20% reduction in hospital readmissions, 25% fewer high-cost imaging services, reduced hospitalizations across a number of disease states, including a 22% reduction in hospitalizations of enrollees with chronic obstruction pulmonary disease. In addition, the program saved $44 million in either direct savings or cost avoidance in FY 2012-13.
Connecticut
- In 2012, Connecticut’s Medicaid program, Husky Health, began a person-centered medical home initiative. Physician practices, federally qualified health centers or hospital outpatient clinics recognized by the National Committee for Quality Assurance as a Level 2 or Level 3 PCMH are eligible for increased reimbursement for primary care services as well as performance-based financial incentives. The program has reduced per person health care spending by 2% and Husky Health has distributed $2.4 million in increased reimbursement or incentive payments to 15 certified medical homes and 1 hospital outpatient clinic.
Illinois
- Illinois Health Connect is a primary care case management program created in 2006 by the Department of Healthcare and Family Services. Illinois Health Connect requires certain Medicaid and Children Health Insurance Program enrollees to select a primary care provider for their medical home. The medical home helps patients get immunizations and other preventive care, prevents service duplication, ensures appropriateness of care, and improves care quality. Primary care providers receive a monthly care management fee for each patient for whom they are responsible and are also eligible for annual bonus payments. From 2007-2010, Illinois Health Connect saved the state $237 million, reduced hospitalizations by 18%, reduced ER visits by 5%, and significantly improved quality on 9 out of 10 metrics.
Maine
- The state of Maine has a strong, multi-year commitment to strengthening its primary care delivery system and is home to several accountable care organizations (ACOs) participating in the Medicare Shared Savings Program and in the Pioneer ACO model. MaineHealth, a non-profit group of providers and other health care organizations, is participating in the MSSP. Using several intervention strategies, including the patient-centered medical home, MaineHealth ACO saved Medicare more than $19 million in its first performance year and earned more than $9.4 million in shared savings, thanks in part to its 100% quality score. MaineHealth is reinvesting most of its shared savings in the ACO participants to support ongoing infrastructure improvements.
Maryland
- The state of Maryland undertook a bold, comprehensive Multi-Payer Patient-Centered Medical Home Program three-year pilot study in 2011. The pilot included 52 primary care and multi-specialty practices, including private practices and every federally-qualified health center in the state. State law required the participation of the state’s five major fully-insured health benefits carriers, and the Federal Employees Health Benefit Plan, Maryland State Employees Health Benefit Plan, TRICARE, and some private employer plans participated on a voluntary basis. Maryland’s primary care medical home model focused on integrated care plans, chronic disease management, medication reconciliation at every visit, increased access to primary care, same day urgent care appointments, and enhanced communication with providers, such as through email. Participating practices received a per-patient per-month Fixed Transformation Payment (FTP) if they achieved National Committee for Quality Assurance recognition and invested a portion of the payment in care coordination. Primary care practices could also share in a portion of the savings they generate. Early outcomes of this program include reduced hospital admissions for young adults with asthma, increased patient and provider satisfaction, improved access to care, including increased well-care visits among adolescents, and an increase in patients with one or more visits to their primary care physician.
Massachusetts
- Massachusetts is a leader in health reform and innovation, and an early adopter of the patient-centered medical home. The state’s Medicaid program, MassHealth, works to transition primary care provider payment towards a patient-centered medical home model, and, in 2012, a state law created a “Model ACO” program under which organizations achieving Model ACO status receive priority recognition from MassHealth, the Group Insurance Commission, and the state’s Health Connector marketplace.One example of a successful medical home in Massachusetts is Partners HealthCare, a participant in the Centers for Medicare & Medicaid Services Pioneer accountable care organization model. In its first performance year, Partners HealthCare achieved total savings of $14.39 million, followed by an additional $3.26 million in savings during performance year 2, while maintaining strong quality scores. Partners credits this success to a focus on population health management, which they describe as investing in services that improve access, help patients navigate the health care system, and provide patients with more information. Key to achieving these goals is Partners’ transformation of all primary care practices into medical homes.
Michigan
- Blue Cross Blue Shield of Michigan currently has the largest network of patient-centered medical homes in the nation, comprised of 4,020 primary care physicians in 1,420 practices. Practices use electronic health records to track patient information and increase patient access to care through extended hours, same-day appointments, and communication via phone or email. Medical homes also focus on prevention, ensuring patients receive annual check-ups and closely monitoring those with chronic conditions. Under this model, primary care and some specialty physicians receive increased reimbursement, called a fee uplift, for certain services if they meet quality and population-based care standards. Blue Cross Blue Shield of Michigan credits the program with reducing hospital admissions by 27.5% for adults with what it calls “ambulatory care-sensitive conditions.” Adult and pediatric ER visits dropped, use of preventive services increased for both adults and children, and composite quality scores increased. This all contributed to a savings of $26.37 per member per month from 2009-2010, and total cost savings of $155 million from 2008-2011.
Minnesota
- In 2010, Minnesota established state criteria for patient-centered medical home certification. This Health Care Homes program became a statewide, multi-payer program with 10 commercial payers, Medicaid, and Medicare, serving 3.3 million Minnesotans through 322 certified health care homes. Participating providers are eligible for care coordination payments from both Medicaid and Medicare, and may also be eligible for quality-based incentive payments. HealthPartners, a participating payer, reported 39% fewer ER visits, 24% fewer hospital admissions, a 40% reduction in readmission rates, a 30% reduction in length of stay, and a 20% reduction in inpatient costs. The Minnesota Department of Health reported that costs for Medicaid Health Care Home enrollees were 9.2% lower than costs for similar Medicaid enrollees not linked to a Health Care Home.
Missouri
- Utilizing Section 2703 of the Affordable Care Act, which allows states to design patient-centered medical homes to provide care coordination to Medicaid beneficiaries with chronic conditions, Missouri requested and received approval to utilize health care homes for Medicaid beneficiaries with mental illness and for beneficiaries with at least two specific chronic conditions. The ACA provides state Medicaid programs with enhanced federal funding for the first two years of a health homes program, which Missouri will use to support participating practice’s care management activities through a per member per month payment. Early results from the health home program include a 12.8% reduction in hospital admissions and an 8.2% reduction in ER use. Improvements were also noted in diabetes control, patient follow-up and medication reconciliation following a hospitalization, and in blood pressure levels in patients with hypertension. The program is credited with a reduction of $127.55 per member per month solely in hospital and ER use costs, and a total cost savings to Medicaid of more than $27 million in the first year.
Nebraska
- Blue Cross and Blue Shield of Nebraska created a patient-centered medical home called Primary Blue. Primary Blue’s mission includes timely access to a primary care physician, a continuous physician-patient relationship, meeting the majority of a patient’s needs in one office, and coordinated, proactively monitored care. Primary Blue focuses on chronic disease management and preventive services. Physicians receive a care management fee and are eligible for outcomes-based bonus payments. In its first year, Primary Blue patients experienced 10% fewer hospitalizations and 27% fewer ER visits.
New Hampshire
- Cigna’s collaborative accountable care initiative is a partnership with Granite Health Network (GHN), a consortium of five chartable, integrated health care delivery systems, to improve health, affordability, and patient experience. GHN participants coordinate and monitor all aspects of an individual’s care and are compensated by Cigna for these services. Participants are also eligible for outcomes-based bonus payments if they meet quality and cost targets. Registered nurses serve as clinical care coordinators and are integrated into the care delivery team to assist patients in navigating the health care system. Cigna reports that the principles of the patient-centered medical home are the foundation of the collaborative accountable care initiative and were adopted by participating physician practices. In its first year, the accountable care collaborative decreased ER use by 4%, reduced advanced imaging use by 7%, and achieved a medical cost trend 1.2 percentage points below the New Hampshire market.
New Jersey
- In 2011, Horizon Blue Cross Blue Shield of New Jersey (BCBSNJ) partnered with the New Jersey Academy of Family Physicians and eight primary care practices to launch the state’s first comprehensive, statewide patient-centered medical home initiative. Under this initiative, physicians, nurse care coordinators, and other practice staff work as a team to coordinate care for Horizon BCBSNJ patients in their practice. The Horizon initiative currently boasts more than 900 practices with more than 3,700 physicians serving more than 200,000 patients. The initiative has reduced ER visits and hospital admissions while improving diabetes control, cholesterol management, and use of preventive services—and producing 2013 cost savings of $4.5 million. On January 1, 2015, Horizon’s program was expanded to Blue Cross Blue Shield organizations in other states.
New York
- Residents of the Washington Heights-Inwood section at the northern tip of Manhattan face numerous social and cultural barriers and experience disproportionately higher rates of chronic disease. Recognizing that the health needs of this disadvantaged community were not being met, New York-Presbyterian Hospital partnered with Columbia University Medical Center and community providers to reduce individual and population health disparities. The care model centered on converting seven ambulatory care centers into National Committee for Quality Assurance Level 3 patient-centered medical homes (PCMHs), which earned them increased reimbursement rates from New York’s Medicaid program. The medical home team included new, culturally competent and often bilingual front line workers from the community, whose backgrounds were similar to many of the patients served by the medical home. In addition, the New York-Presbyterian Regional Health Collaborative, as the partnership is known, took the PCMH model a step further, linking the medical homes to other providers and community-based services to create a “medical village.” This model of care reduced ER visits by 29.7%, reduced hospitalizations by 28.5%, achieved increased patient satisfaction scores across a host of measures, and yielded a short-term return on investment of 11%. A large part of the financial gain was due to increased Medicaid reimbursement to the medical homes, but the reduction in ER visits contributed $381,000 in cost savings.
North Carolina
- As one of the first statewide patient-centered medical home networks in the country, Community Care of North Carolina (CCNC) is a model for community-based primary care teams. This public-private partnership brings together regional networks of health care providers to deliver coordinated care using the medical home model. It is a multi-payer initiative, involving Medicaid, the state employee health plan, Blue Cross and Blue Shield of North Carolina, and Medicare (through the Multi-payer Advanced Primary Care Practice program). CCNC aims to improve care, reduce costs, connect every Medicaid beneficiary with a medical home and community network of supports, and develop local systems to improve chronic disease management. Community networks and primary care providers receive a per-member per-month payment to fund care management and coordination activities. An independent study estimates that CCNC saved the Medicaid program more than $980 million during fiscal years 2007-2010.
Utah
- Hill Air Force Base, outside of Ogden, Utah, experienced cost savings and improved care quality after implementing a patient-centered medical home (PCMH). Hill was a project site for the Department of Defense’s (DOD) Tri-Service PCMH project to coordinate care at all DOD primary care practices. Using a team-based approach, primary care practices create personalized care plans for each patient, improve access to care, and provide care management services. The PCMH project improved blood sugar control for 77% of participants with diabetes, saving the Air Force an estimated $300,000 per year, and maintained symptom control at or above 98% for patients with asthma. Air Force personnel credit the PCMH project with helping to drive down health care costs for two consecutive fiscal years.
Vermont
- Vermont’s health care reform is guided by the Blueprint for Health, a statutory, state-led initiative to transform primary care, and health care more broadly, both in terms of delivery and payment. The multi-payer model includes patient-centered medical homes (PCMHs), multi-disciplinary community health teams (CHTs), self-management support programs, comparative reporting from statewide data systems, and a focus on continuous improvement and learning. In addition to usual, fee-for-service payments, PCMHs receive a per-member per-month payment if they have a qualifying score on the National Committee for Quality Assurance’s PCMH standards, with higher scores yielding higher payments. CHTs receive capacity payments to support their salaries and expenses of $350,000 for every 20,000 patients. The Blueprint model reduced hospitalizations for commercially insured adults and for adult and pediatric Medicaid beneficiaries. Commercially insured adults and children covered by Medicaid also experienced fewer ER visits. Expenditures fell for commercially insured and Medicaid insured patients across all ages, with savings ranging from $200-$586 per participant per year.
