Report Published March 30, 2015 · Updated February 3, 2016 · 16 minute read
Make Telehealth an Easy Way for Patients to Get Care

Feeling sick doesn’t restrict itself to regular office hours. Why should health care? Under stress, and often after regular business hours, patients experiencing acute symptoms make snap decisions to go to the emergency room because they are fearful and have few other choices. Or they may delay needed care until “normal business hours.” This results in exorbitantly high medical costs for patients who actually only needed non-emergent care.
What if people could get care anytime from the comfort of home? Available 24 hours a day, 7 days a week, personalized “telehealth” sessions allow patients to connect to providers via phone or a webcam and discuss their current conditions. Through these virtual sessions, a nurse or physician evaluates the patient using real-time audio and video tools and determines the next steps for care that can range from monitoring symptoms to issuing a prescription, or in some cases, referring the patient for follow up care. For this reason and others, telehealth is becoming more and more invaluable to patients in some parts of the country where state law allows it. In addition to increasing patient satisfaction, implementing telehealth on a national scale would also save money by shifting the cost of care from high-cost settings like emergency rooms to the much lower cost of telehealth services. But persistent barriers to telehealth remain in states and throughout Medicare and Medicaid that prevent telehealth from keeping the promise of better health and better cost.
This idea brief is one of a series of Third Way proposals that cuts waste in health care by removing obstacles to quality patient care. This approach directly improves the patient experience—when patients stay healthy, or get better quicker, they need less care. Our proposals come from innovative ideas pioneered by health care professionals and organizations, and show how to scale successful pilots from red and blue states. Together, they make cutting waste a policy agenda instead of a mere slogan.
What is Stopping Patients From Getting Quality Care?
Telehealth is an important tool that can be used to educate patients, facilitate patient-provider communication, and engage patients more fully in their care outside of the doctor’s office.1 Specifically, telehealth is defined as the “use of electronic information and telecommunications technologies to support long-distance clinical health care, patient and professional health-related education, public health and health administration.”2 It encompasses a broad range of activities, such as videoconferencing, remote patient monitoring, streaming media, and terrestrial and wireless communications.3 In short, telehealth aims to provide a way to receive care no matter the patient is. As a result, it has significant potential to be an important tool for providers trying to coordinate care across settings.
The problem is straightforward: telehealth adoption has lagged behind its promise due to regulatory and payment barriers that haven’t caught up to new technologies and payment methods. To begin with, no two states define or regulate telehealth in the same way.4 Often, there are even inconsistencies on telehealth policies within states.5 Medicaid policies defining and paying for telehealth also differ across states. Federal law including Medicare has multiple definitions of telehealth that severely restrict its use and reimbursement. And private plans do not consistently reimburse for telehealth across states
Many states also have outdated licensing regulations that impede the adoption of telehealth programs—especially for health systems that operate across state lines. For instance, most states require physicians to have a license in the originating site’s state and others require providers using telehealth to have a license in the state where the patient is physically located.6 Meanwhile, state medical boards in 11 states issue special purpose licenses, telemedicine licenses or certifications, or licenses to practice across state lines.7 With each state regulating telehealth differently, providers are virtually guaranteed to face additional licensing or paperwork if they seek to deliver any care via telehealth technologies.
Despite these hurdles, 42% of hospitals have telehealth capabilities, but it tends to be limited.8 Those hospitals with the greatest technological capabilities—such as a cardiac ICU, are part of a larger system, or are teaching hospitals—were more likely to have adopted some form of telehealth.9 Hospitals in rural areas were also more likely to have telehealth capabilities. Importantly, there were significant relationships between telehealth adoption and state policies.10 In particular, state policies requiring out-of-state providers to have special licenses reduced telehealth adoption, and policies requiring private health plans to reimburse for telehealth were associated with greater adoption.11 Telehealth adoption is driven by the need to increase access to care for rural residents, but also for competitive and strategic reasons—especially in markets where there is a need to deliver more efficient care to complex patients.12
Varying (or nonexistent) payment for telehealth across plans has also impeded adoption. For instance, Medicare only reimburses for telehealth services when strict criteria are met, such as patients having to be in a designated Health Professional Shortage Area or having to travel to a telehealth facility rather using their own computer or portable device. At the same time, 46 state Medicaid programs reimburse for at least some type of telehealth services,13 but only 21 states require private plans to provide coverage for telemedicine services that is comparable to coverage for face-to-face services.14 The historical reticence to pay for telehealth is understandable—in a fee-for-service system it could very likely drive up utilization and costs. However, telehealth services are often less expensive than face-to-face services. Moreover, at a time when the health care system is trying to move away from fee-for-service and towards value-based payments that require providers and patients to engage more directly to manage chronic disease, avoid use of unnecessary services, and prevent disease altogether, it needs access to technologies that can facilitate flexible interactions and transmit and share data on a patient’s health status.
Finding ways to bring care to patients in new ways, to support behavior change, and to engage individuals in their health can be a more cost-effective strategy than simply providing more (or different) health care services in many cases. Telehealth is an existing technology that has shown the ability to help accomplish these objectives, but it needs to be far more widely available to providers and patients.
Where Are Innovations Happening?
Telehealth is intended to complement traditional health care services—ambulatory and hospital-based care that are provider-centric—and help create a delivery system that is patient-centric by extending outside of provider offices.15 Throughout the country, there are a number of examples of telehealth expansion to specific patient populations (especially those with chronic illnesses) that are also demonstrating impressive results.

- LiveHealth Online is an example of a telehealth platform that connects patients with physicians and providers at times when appointments may not be available.16 Anthem health plans are offering LiveHealth Online services to members as an alternative to emergency room and urgent care, which cost more.17 Enrollees can contact providers via live audio/video and chat in the convenience of their homes or workplaces.18 Typical telehealth encounters through LiveHealth Online are for colds and related viruses, allergies, infections, and wellness questions.19 The telehealth encounter may be shared (with patient permission) with a patient’s primary care doctors to facilitate care coordination.20 LiveHealth Online demonstrates the value that private plans are discovering in using telehealth by increasing off-hours access to providers—to avoid potentially costly emergency room and urgent care visits.
- Project ECHO (Extension for Community Healthcare Outcomes) started at the University of New Mexico in 2003, and since has expanded nationally and globally. Project ECHO started as a way to connect patients in rural New Mexico with Hepatitis C to specialty care. Today, the program is used to treat numerous conditions including diabetes, asthma, rheumatoid arthritis, behavioral health, and chronic pain. Project ECHO links primary care practices to specialty treatment so that front-line providers have the necessary knowledge and support to manage complex conditions.21 By linking specialists to primary care practices in rural and/or underserved communities, Project ECHO is helping address disparities in care, rising costs, inefficiencies in delivery systems, and slow diffusion of best practices.22 In short, the program aims to do more without necessarily spending more money.
- Arkansas e-Link started in 2003 as a support mechanism for high-risk pregnancy consultations. Today, the program covers multiple medical specialties and patient populations, including asthma care, pediatric cardiology, gynecology, and mental health.23 The program’s primary aim is to provide interactive video medical consultations for patients, local providers, and remote specialists; however, the network is also used for continuing medical education and support services.24 One example of how Arkansas e-Link is transforming care is with its mobile application for pre-teens and teens with asthma. Asthma management assistance is provided via text message tips and reminders, as well as daily tracking of peak flow and asthma symptoms.25 The program has led to significant improvements—with mean scores on an asthma control measure moving from uncontrolled to controlled.26 Better controlled asthma is likely to lead to reduced admissions or trips to the doctor’s office—keeping care in lower cost settings.
- The Veterans Administration (VA) provides another successful example of widespread telehealth adoption. In Fiscal Year 2012, the VA provided nearly 1.5 million telehealth episodes of care using home telehealth, clinical video telehealth, and store and forward telehealth technologies. The impact of this extensive telehealth network is impressive. In Fiscal Year 2012, 35% of veterans enrolled in home telehealth services, which involves monitoring patients and managing diseases in home and with the use of mobile devices for acute and chronic care management as well as health promotion and disease prevention, were able to remain in their homes as opposed to transitioning to long-term institutional care.27 The VA provides a model for how comprehensive home telehealth services can keep patients in the community.
- HealthCare Partners, operating in Southern California, Florida, and Nevada, launched a particularly successful remote patient monitoring (RPM) program for patients 65 years or older with chronic conditions, including chronic obstructive pulmonary disease (COPD). The program used a telephone-based home monitoring system to reduce emergency room visits and hospital admissions, gave providers clinical parameters to manage chronic conditions, and provided participants with user-friendly technology to remain in their preferred residence and engage them in managing their health. In the first year alone, the program demonstrated a return on investment of 1.3—saving $1.30 for every $1 invested.28 For years two through five of the program, the rate of return is projected to increase steadily from 7.2 to 18.9. Total returns per patient were estimated to be $4,388, mostly due to reduced hospital admissions.29 The high rate of return is at least partially attributable to specific program features including the use of interactive voice response (IVR) technology and opt-out patient enrollment.
How Can We Bring Solutions To Scale?
The growing evidence on the potential for telehealth to improve patient outcomes and reduce costs has led to legislative changes and continued efforts to further expand access to telehealth and its related technologies. Most recently, the Medicaid and CHIP Reauthorization Act of 2015 (MACRA) law includes initial steps to lift payment and other barriers to telehealth use for providers participating in alternative payment models (APMs).30 These initial policy changes serve as the basis for additional steps federal policymakers, state governments, and private health plans can take to expand telehealth use across payers and populations. Available policy levers for increasing access to telehealth include eliminating restrictive state policies, further modifying Medicare and Medicaid payment policies for telehealth to accelerate adoption, harmonizing payment policies across public and private health plans, and directing telehealth use with populations served via value-based payments and APMs.
First, eliminating restrictive state policies could significantly increase the use of telehealth—especially at a time when providers are seeking high-value ways to coordinate care for patients across settings. For health systems that operate across state lines or rural states, additional licensing requirements are serious barriers to telehealth adoption. Eliminating requirements for out-of-state providers to have special licenses to provide telehealth services across state lines (if they are already licensed in the state where the service is originating) would be helpful. In addition, there are also varying credentialing requirements at different facilities. Providers have to be credentialed not only at the site where they are originating the telehealth service, but also the site where the patient is in many cases. Licensing and credentialing requirements could be harmonized across states by creating and requiring a special purpose license to cover all telehealth interactions within and across state lines.31 State Boards of Medicine can take a first step by adopting the model policy for telemedicine developed by the Federation of State Medical Boards.32
Second, Medicare and Medicaid must modernize payment policy for telehealth and leverage APMs to accelerate the adoption of technologies that engage patients in their care and avoid the use of intensive, often costly, services. Medicare is the most significant lever for changing payment policy in health care. The move to value-based payments and APMs was greatly accelerated as a result of new Medicare programs, such as the Hospital Readmissions Reduction Program and the Hospital Value-based Purchasing Program, among others. In the same way, modernizing Medicare payment for telehealth services so that it is responsive to the care coordination challenges providers face in today’s market could facilitate private health plans to follow suit. It would also give providers a clear signal on how plans are committed to telehealth so they are willing to make the necessary upfront investments.
Medicare policy has been shifting in recent years, but there is potential to do much more. For instance, Medicare expanded its list of covered services to include seven new telehealth services, including psychotherapy, and also included provisions for paying for remote monitoring of chronic conditions.33 However, beneficiaries must still be in a HPSA in order for providers to bill for services and they must travel to a telehealth site, known as an originating site, in order to use the service. In 2015, MACRA lifted payment and site origination barriers, among others, to promote the use of telehealth and related technologies for providers participating in APMs.
Congressional activity is continuing to build on these initial policy changes to further accelerate adoption of telehealth technologies that show promise in improving outcomes and reducing costs. For instance, Senators Brian Schatz (D-HI), Roger Wicker (R-MS), Thad Cochran (R-MS), Ben Cardin (D-MD), John Thune (R-SD), and Mark Warner (D-VA), and Representatives Diane Black (R-TN), Peter Welch, (D-VT), and Greg Harper (R-MS) have introduced the CONNECT for Health Act to increase access to telehealth and RPM through targeted changes to Medicare payment policy.34 This legislation builds on previous efforts, including the Telehealth Modernization Act proposed by Reps. Doris Matsui (D-CA) and Bill Johnson (R-OH) and the 21st Century Cures initiative led by Reps. Fred Upton (R-MI) and Diana DeGette (D-CO).35 The CONNECT for Health Act legislation would expand the telehealth provisions in MACRA by:
- Providing payment for care management through telehealth and RPM services for those providers eligible for the merit-based incentive program (MIPS), which adds bonuses and penalties to Medicare fee-for-service payments and those participating in APMs; and
- Covering and paying for RPM services in fee-for-service Medicare for patients with 2 or more chronic conditions and with a history of hospitalizations or ED visits in the prior year.
As value-based payments evolve to increase provider risk-sharing, there is decreasing incentive to overutilize services. Directing the use of telehealth in accountable care organizations (ACOs), bundled payments, or patient-centered medical homes (PCMHs) where providers are incentivized to provide high-quality care as efficiently as possible could be an important way of increasing its use across the care continuum. It would also protect against concerns from providers that traditional revenue from face-to-face visits and reimbursed services will decrease.36
Last, these policy and payment changes should be extended to Medicaid programs to allow providers to fully leverage and apply telehealth technologies to improve outcomes and reduce costs. There is wide variation in telehealth coverage and payment across Medicaid programs. For instance, some states only pay for live video technology for behavioral health services, while others will pay for a wide range of specialties. In addition, there are differences across state Medicaid programs in the type of services and providers that are reimbursed, the location of the patient, and the location of the provider.37 Remote patient monitoring is another highly cost-effective telehealth technology with restrictive use.38 Only 13 state Medicaid programs reimburse for remote patient monitoring in some form—usually restricted to home health agencies and for specific conditions.39 Medicaid policy for authorization and payment for telehealth, including RPM, could be modeled after the CONNECT for Health Act legislation, which allows for coverage and payment for telehealth services within the context of APMs and with targeted patient populations in fee-for-service.
Potential Savings
Based on a phased-in approach to expanding access to telehealth services in Medicare, the ten-year federal savings from 2017-2026 are projected to be $1.8 billion.40 The chart below shows the year-by-year budget impacts over the ten-year budget window.
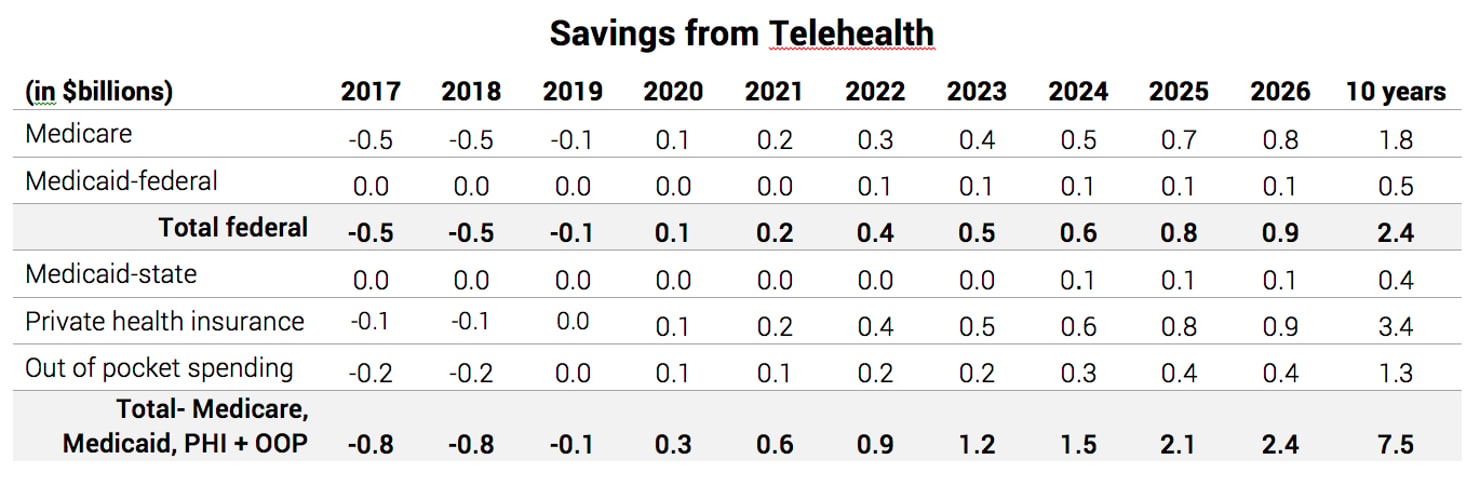
- These budget estimates are based on the following Medicare policies, which correspond to provisions in the CONNECT for Health Act legislation:
- Coverage for telehealth, including RPM from September 2016 until December 2018 for providers who will be eligible for MIPS starting in 2019; Coverage for telehealth, including RPM for providers participating in APMs starting in Fiscal Year 2020; and
- Medicare coverage for RPM starting six months after for all fee-for-service physicians and practitioners for beneficiaries, MIPS and APM providers starting in fiscal year 2020. In this provision and the two above, RPM coverage will be for chronic conditions for which the Centers for Medicare & Medicaid Services (CMS)’ Actuary determines there will be no net increase in Medicare expenditures resulting from the proposals.
The first policy, expanding telehealth and RPM service coverage and payment to those providers qualifying for MIPS, cost Medicare $1.1 billion over 10 years. However, the second policy, which targets providers in APMs saves $2.2 billion over 10 years. The third policy, which covers only RPM, but for all providers would produce, $3.0 billion in savings. Together, the policy changes produce a net deficit reduction of $1.8 billion over 10 years after eliminating the overlap between policies two and three. It is also important to note that Medicare would reimburse only for RPM for beneficiaries with chronic conditions for which the CMS Actuary determines there will be no net increase in Medicare expenditures.
The total federal and state Medicaid savings of $0.9 billion over 10 years would be the result of applying similar policies at the state level beyond what is already in place to varying degrees in several states.41


