Report Published May 24, 2023 · Updated June 14, 2023 · 12 minute read
Stop Hospitals from Padding Bills for Routine Care
Darbin Wofford & David Kendall

Takeaways
Hospitals have been buying up physician practices across the country. Over half of all US physicians are now employed by hospitals or large health care delivery systems. The result: increased prices for outpatient services.
One of the most pernicious examples of this is the dreaded “facility fee,” where hospitals buy a physician practice only to be able to charge an extra fee for performing the same service. These higher prices drive up out-of-pocket costs for patients, spending for Medicare, and premiums for private coverage.
In this report, we recommend policies to move towards a site-neutral payment system that would tie prices to the value of the care being provided, rather than who owns the location of care.
Kyunghee Lee, a 72-year-old retiree living outside Cleveland, was outraged by the bill she received for her annual treatment for painful arthritis in her fingers. For years, the bill had been about $30, but this time it was $355. 1 The total bill came to $1,394, which included for the first time a $1,262 facility fee. The only difference was that the hospital had reclassified the care as an outpatient hospital visit instead of a physician office service. Unfortunately, Kyunghee isn’t alone. For the last several years, hospitals have been padding bills with facility fees for services that can be delivered in a physician’s office for far less.
Medicare and private health plans have historically paid more for medical services delivered by hospitals for outpatient care. Hospitals are now taking advantage of that difference by buying up physician practices and then charging facility fees, like Kyunghee received for her treatment. They also hide these actions from health plans by claiming newly purchased physician practices are part of an outpatient department, even when the physical location of the practice hasn’t changed. Some patients are now seeing a doctor in their office and receiving a bill from a hospital, which includes a facility fee.
The solution is simple: tie prices to the value of the care being provided rather than who owns the location of care. The technical term for this is site-neutrality. This report explains how hospital consolidation has increased prices for outpatient services and patients. It then shows how to make site neutrality universal and reap significant savings for consumers and the broader health care system.
This report is part of a series called Fixing America’s Broken Hospitals, which seeks to explore and modernize a foundation of our health care system. A raft of structural issues, including lack of competition, misaligned incentives, and outdated safety net policies, have led to unsustainable practices. The result is too many instances of hospitals charging unchecked prices, using questionable billing and aggressive debt collection practices, abusing public programs, and failing to identify and serve community needs. Our work will shed light on issues facing hospitals and advance proposals so they can have a financially and socially sustainable future.
The Problem: High Prices for Routine Care
Hospital consolidation has increased prices for outpatient services, which drives up costs for patients. On top of that, hospitals lack incentives to deliver better care at lower costs.
Consolidation has increased prices for outpatient services.
Hospitals have been buying up physician practices across the country. Over half of all physicians in the United States are employed by hospitals as of 2022, a trend that has been on the rise since 2012.2
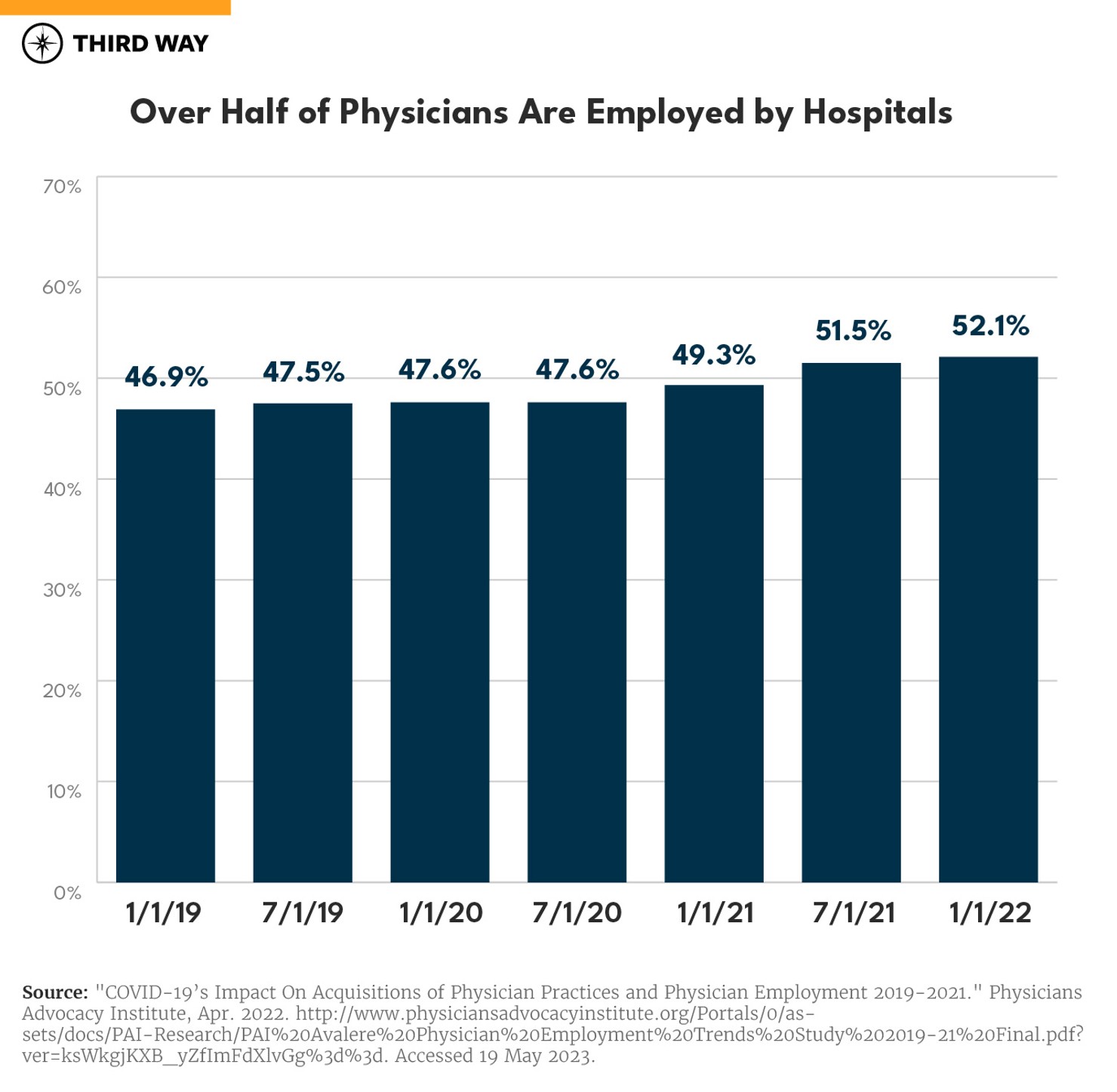
With consolidation, hospital systems increase their prices without adding any value to the medical services they provide. Hospitals are doing this, in part, by billing higher hospital rates for services at newly acquired physician offices. When a hospital buys a physician’s office, it becomes part of the hospital outpatient department, even if its physical address has not changed. After a hospital acquires a physician’s office, prices increase an average of 14%.3
The difference in prices between outpatient departments and physician offices varies depending on the type of service. For example, a chest X-Ray in a hospital outpatient department costs Medicare $91.61, versus $26.65 in a physician’s office.4
The Medicare Payment Advisory Commission (MedPAC), which advises Congress on Medicare policy, identified 57 services where it would be appropriate for services provided in an outpatient department to be paid at a physician office rate by Medicare.5 Higher prices for these services resulted in $6.6 billion in overpayments to Medicare.6
Higher prices drive up costs for patients.
Medicare payments for hospital outpatient services are projected to grow faster than any other service over the next decade at 87%. Comparatively, physician payments through Medicare are projected to grow by 22%. Growth in Medicare’s spending on outpatient departments also outweighs growth in other goods and services, including prescription drugs, hospitals, home health care, and skilled nursing facilities.7
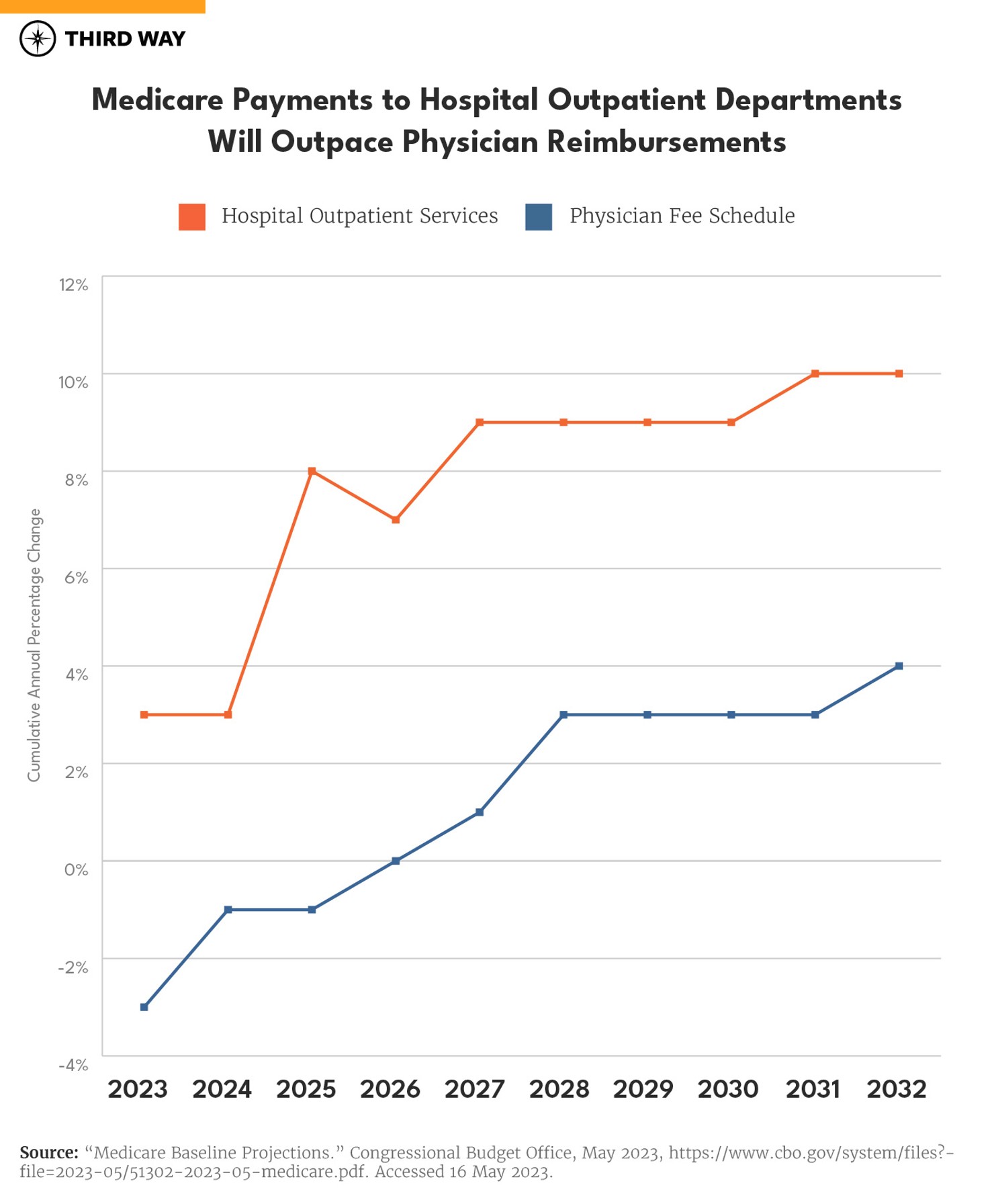
For seniors enrolled in Medicare, these higher prices result in higher out-of-pocket costs. Seniors are typically responsible for 20% of the cost of services being provided. According to the Centers for Medicare and Medicaid Services (CMS), “this additional hospital copayment means you may pay more for an outpatient service you get in a hospital than you’d pay if you got the same service in a doctor’s office.”8
In addition to the 20% copayment, the higher cost of hospital outpatient services translates into more spending by Medicare’s medical insurance (Part B) program. This means higher premiums for seniors along with higher copayments, leading to a $1.7 billion burden on seniors in 2019 alone.9
In the private insurance market, acquisition of physician offices increases their negotiating power over insurers. As hospital systems become more dominant in a geographical area, insurers lose leverage in their contract negotiations, resulting in higher prices. Those high prices translate into higher premiums for private coverage and more out-of-pocket costs for patients through facility fees.
As telehealth utilization has grown exponentially from pre-COVID-19 pandemic levels, facility fees for telehealth services have become increasingly common.10 Facility fees are billed to patients utilizing telehealth services if their provider is part of a hospital system, despite the patient never setting foot within a hospital’s facility. When Brittany Tesso in Colorado had a telehealth appointment for her son’s speech therapy in 2021, she received one $676 bill for the appointment and a second $847 bill for the facility fee. 11
Overbilling for telehealth services has led several states to ban facility fees attached to telehealth services. Facility fees for telehealth services also occur in Medicare, where providers are permitted by the program to bill patients approximately $27 per telehealth visit.
Hospitals lack incentives to deliver better care at lower costs.
The financial incentive for hospitals to purchase physician practices in pursuit of charging higher prices is ultimately the result of fee-for-service health care. Fee-for-service is the prevalent payment model in the United States in which medical providers, such as hospitals and physicians, charge for separate services. Because each service receives its own payment, providers have a strong incentive to inflate prices and provide as many services as possible.
Hospitals maximize their revenue by buying physician offices and billing for additional services. As hospitals consolidate with other hospitals as well as physicians, they can use their market power to dictate prices.
Hospitals counter that higher prices in outpatient department settings are warranted due to their facilities treating sicker patients. While this may be true for inpatient care, in which Medicare adjusts its reimbursements based on how sick a patient is, primary care, tests (such as MRIs), and minor procedures do not cost the facility more to treat patients with diagnoses unrelated to the treatment.12 Services should be reimbursed based on the provided treatments, not unrelated diagnoses.
The Solution: Site-Neutral Payments
Prices paid for medical services should reflect the value of the care being provided, not whether the location of service is owned by independent physicians or a hospital. The technical name for this solution is called site-neutral payments, which has been supported by the Obama and Trump Administrations.13 Site-neutral payments would provide financial relief for patients through out-of-pocket savings and decrease the overall cost of coverage in both Medicare and commercial health insurance.
Medicare took an initial leap towards site-neutral payments when Congress passed the Bipartisan Budget Act of 2015. The law established site-neutral payments under Medicare for certain outpatient departments located away from the hospital. This was a significant step towards reducing outpatient costs as many services have shifted from inpatient to outpatient settings. However, the law applied only to new outpatient locations and exempted physician practices that were converted into outpatient departments.14 The law did not apply to on-site locations, where the outpatient department is located within the hospital’s campus.
Broadening site-neutral payment policy would require three steps:
First, require hospitals to disclose the physical location of the site of care. Congress can create this kind of transparency by requiring bills from off-site hospital outpatient departments to contain a different provider identifier than the hospital. For example, legislation introduced by Representatives Kevin Hern (R-OK) and Ann Kuster (D-NH), the Facilitating Accountability in Reimbursements (FAIR) Act, would create these unique identifiers for providers in Medicare and private insurance.15 Today, hospital departments located away from the actual hospital site will often use the hospital’s identifier for billing purposes, giving the impression that care is being delivered on the hospital premises, rather than another location. A separate identifier would allow payers to apply the appropriate reimbursement rate to outpatient services delivered at sites away from the hospital. Transparency would also allow private health plans to halt facility fees.
Second, expand site-neutral payments in Medicare. This step would extend Medicare’s current site neutrality payment requirements to include outpatient departments that are located on the hospital campus. Requirements should be extended to all hospital outpatient departments, regardless of when they were built or whether they were an acquired physician practice. These requirements would only be applied to appropriate services, determined by CMS. For example, in MedPAC’s June 2022 report, 57 services were identified for which it would be reasonable to align payment rates.16 Again, this policy had the support of previous Democratic and Republican administrations and has bipartisan support on the Hill.17 Senators Mike Braun (R-IN) and Maggie Hassan (D-NH) have introduced the Site-based Invoicing and Transparency Enhancement (SITE) Act that would expand Medicare’s current site-neutral requirements, along with requiring site disclosures.18
Third, encourage value-based payments. Shifting away from fee-for-service towards value-based care would lower prices, improve quality, and create a more equitable health care system. As part of site-neutral policies, Congress should increase payments to physicians at the same time it lowers payments to hospitals for the same set of services. Increasing physician payments through Medicare’s physician fee schedule would decrease incentives for selling their practice to a hospital. Additionally, site-neutral policies in Medicare should be delayed by three years for accountable care organizations to allow time for the baseline for payments they receive from Medicare to adjust to the new policies. In general, policies that increase the use of bundled or capitated payments and encourage hospital participation in accountable care organizations that coordinate high-quality care would build on site neutrality. And they would reward hospitals for delivering value-based care to patients and encourage quality over quantity.
The Savings
Moving towards site-neutral payments would result in significant savings for beneficiaries and the Medicare program. According to one estimate, site neutrality would save the federal government between $217 and $279 billion over a decade.19 Because Medicare beneficiaries are responsible for roughly 20% of Medicare Part B premiums and the same share in the total cost of service, reduced Medicare reimbursement for outpatient services would decrease seniors’ costs by $94 billion over the same period. For a patient like Kyunghee, that's $325 in direct savings per visit for treating her arthritis. Some of these savings could be offset with increases in Medicare payments to physicians.
Payment reforms in Medicare would have significant spillover in the commercial market. Because private health plans often set payments using Medicare rates, reductions in Medicare rates would translate into reduced payments from commercial payers for the same services. Reductions in spending by private insurance would lower premiums for both individual market and group health plans.
In addition to the commercial effects of site neutrality in Medicare, transparent billing and bans on facility fees would have a more direct impact on ACA and workplace premiums. Estimates for site neutrality for off-site locations in the private sector would decrease premium and out-of-pocket spending by $80 billion over a decade, with a federal impact of $21 billion in savings. If site neutrality were extended to payments for on-site locations, federal spending on private coverage would decrease by $117 billion and save $458 billion in premium and out-of-pocket spending.20
Conclusion
As hospital costs rise and patients struggle with out-of-pocket costs, high premiums, and medical debt, site neutrality for outpatient services is a crucial way to lower health care costs. Prices should be determined not by the site of service, but the quality of the care being provided.
The savings from site-neutral payments would be significant—lowering costs for patients and helping the government fund other priorities such as permanently extending the improved caps on premiums in the Inflation Reduction Act for people who get coverage through the Affordable Care Act exchanges.
Site-neutral payments also provide a springboard for more policy interventions on out-of-control hospital pricing. Along with revitalized anti-trust regulation and limits on anti-competitive contracting, policymakers can decrease costs across the health care system and increase the affordability of health care in the United States.


