Report Published December 8, 2017 · Updated December 7, 2017 · 8 minute read
Creating a Comprehensive Strategy to Support Family Caregivers

Every day, Angela Goodhope of Mapleton, Iowa, must clean and disinfect her teenage daughter’s central line, a catheter that delivers medicine to treat a rare type of blood cancer.1 The line can get infected and send deadly bacteria into a vein next to her heart. One afternoon, her temperature spiked, which signaled an infection that landed her daughter in an isolation room at the hospital for four days. Antibiotics thankfully cured the infection, but it shook Angela’s confidence in caring for her daughter.
Family caregivers like Angela face complex, stressful tasks, often with minimal training and support.2 They are on the front lines of the care that millions of Americans need every day, and their success can make all the difference in the health and well-being of their loved ones. It can also prevent costly hospitalizations and treatment. A new program pioneered at the Dana-Farber Cancer Institute/Boston Children’s Hospital trains caregivers for several days before a central line is inserted and sends a nurse to the home to support family caregivers.3 Such training has dramatically reduced bloodstream infections stemming from care at home.
But getting support like this nationwide is no small matter. Who exactly is responsible for supporting family caregivers as they assist with activities of daily living (like bathing and dressing), tasks needed to live independently (like shopping and preparing meals), and complex medical/nursing tasks (like wound care and injections)? And what about their health, which often suffers while helping others? Family caregiving is also facing demographic headwinds that threaten to eliminate billions of dollars’ worth of critical care. Addressing these problems will require a comprehensive strategy that can enable communities across the country to improve their support for family caregivers.
This report is divided into two sections. The first section highlights the key challenges facing family caregivers today, and the second section details the proposed solution.
The Key Problems Facing Family Caregiving
- Family caregiving has become more time consuming and stressful as loved ones’ needs increase.
- The number of family caregivers is not keeping pace with demographic changes.
- Without family caregiving, the health and well-being of individuals would be worse and costs would be higher.
1. Family caregiving has become more time consuming and stressful as loved ones’ needs increase.
The United States has 43.5 million adults who serve as family caregivers.4 Their average age is 49–years-old, but people of all ages serve as family caregivers. They may have a rewarding and meaningful experience, but also one which is growing more demanding and stressful.
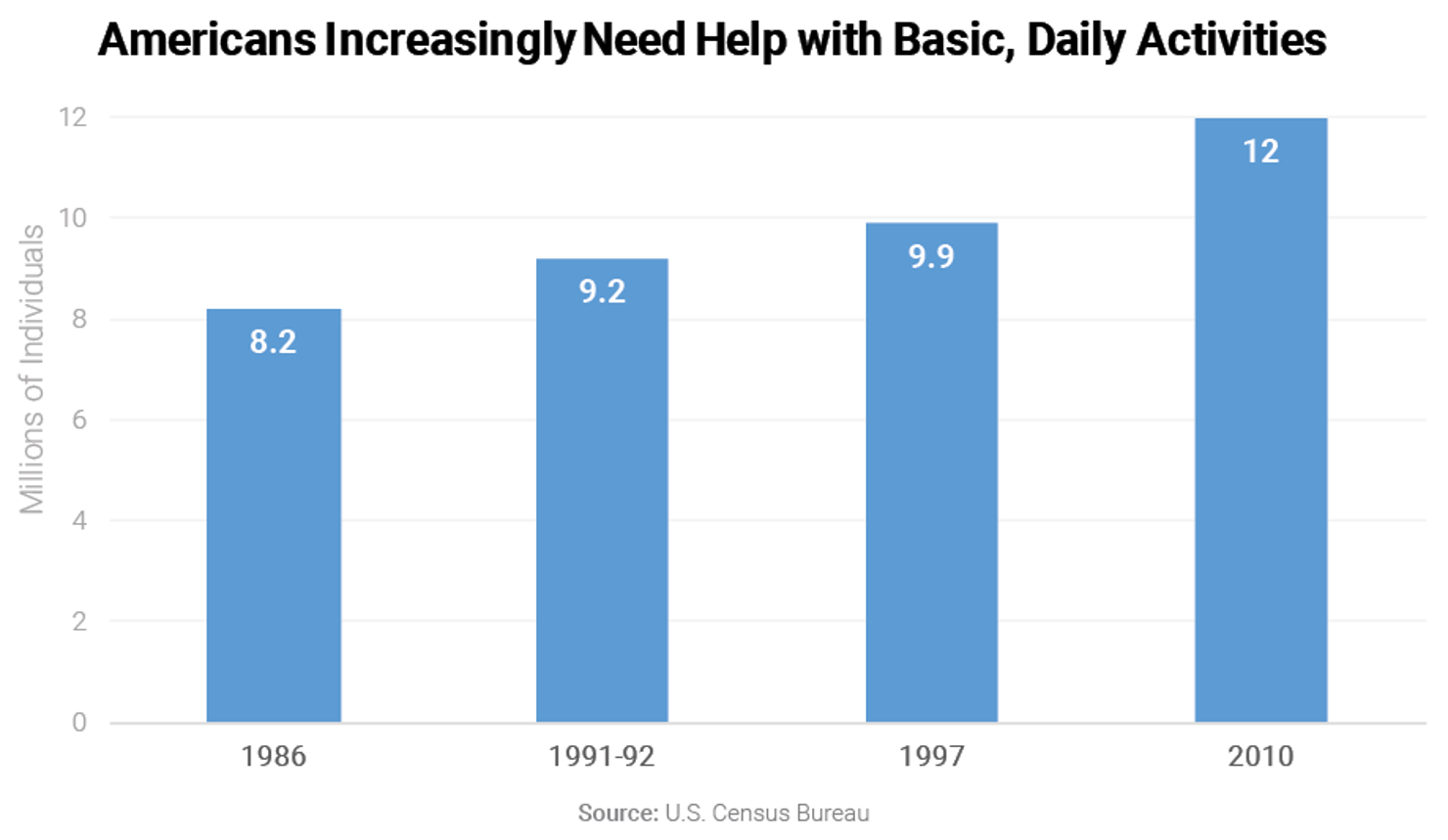
The overall need for family caregivers is growing, as the number of Americans who need personal assistance with at least one daily activity has increased from 8.2 million (4.4% of the population) to 12 million (5% of the population) from 1986 to 2010 (the latest data available).5 Of those individuals requiring assistance, the number and percentage with greater care needs is also increasing. The number of Americans ages 15 and older who need personal assistance with three or more daily activities while living with others or independently has increased from 4.6 million to 5.6 million, which is an increase from 2.2% to 2.3% of the population from 1997 to 2010 (no comparable data is available before 1997 or after 2010).6
In part due to the higher needs of care recipients, caregiving is often a full-time job. In 2015, 23% of family caregivers spent more than 40 hours per week providing care.7 Indeed, those caregivers spent 71 hours per week on average providing care.8
In 2014, 57% of family caregivers reported performing medical or nursing tasks like injections and tube feedings.9 Partly due to that responsibility, an increasing number of family caregivers find their experience to be highly stressful.10 In 2014, nearly 40% of caregivers to adult care recipients ranked the emotional stress of caregiving as a four or five on a five-point scale.11 Emotional stress levels are higher among individuals caring for those with a mental health issue, like Alzheimer’s or dementia, or a long-term physical condition.12 One-third of caregivers say that coordinating care for a loved one with three or more conditions is difficult.13
The physical toll on family caregivers is substantial. According to the National Academies of Sciences, Engineering, and Medicine:
Substantial evidence indicates that family caregivers of older adults are at risk compared to non-caregivers; they have higher rates of depressive symptoms, anxiety, stress, and emotional difficulties. Evidence also suggests that caregivers have lower self-ratings of physical health, elevated levels of stress hormones, higher rates of chronic disease, and impaired health behaviors.14
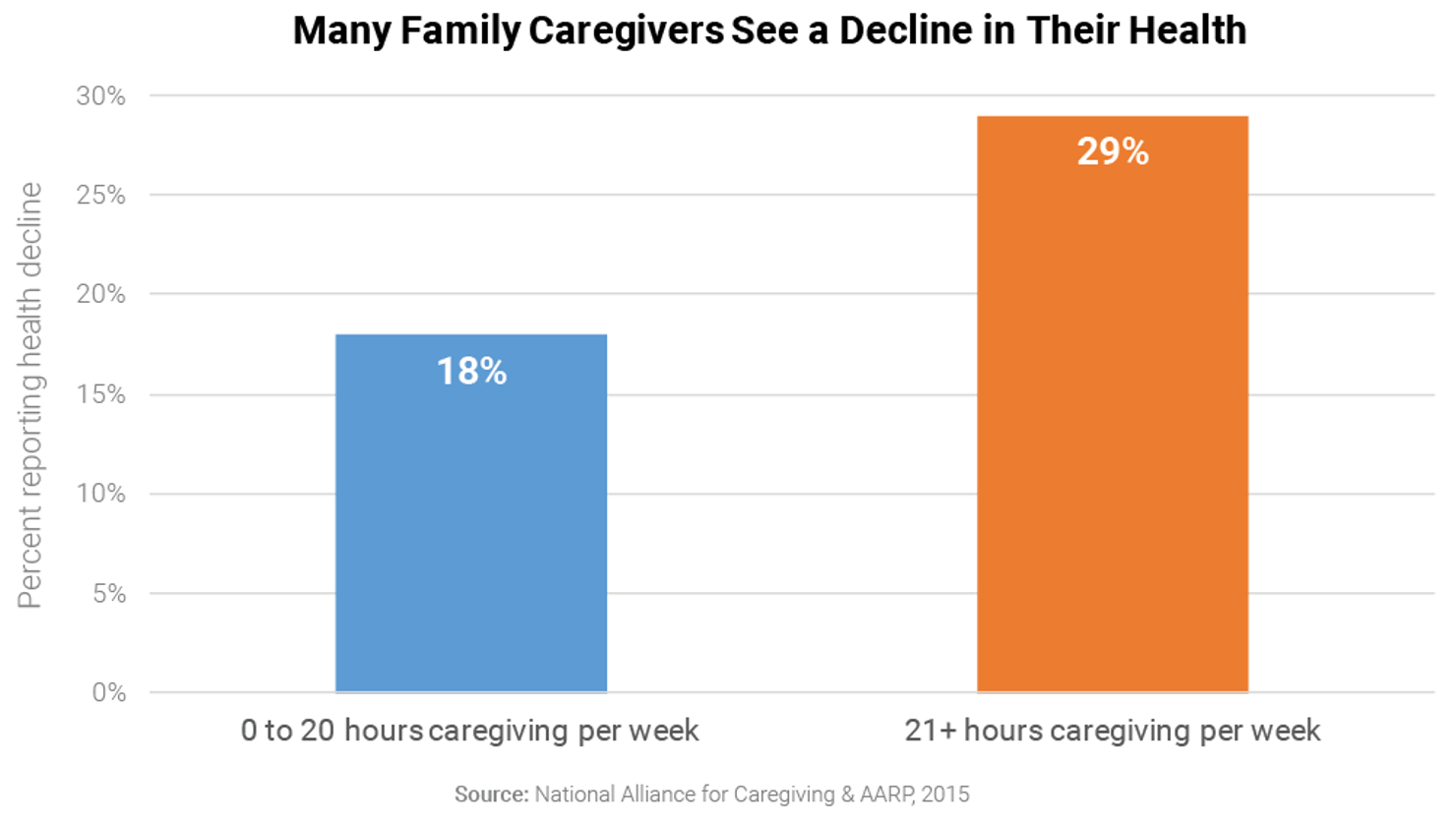
The health impact on family caregivers stems in part from neglecting their own health and well-being as they are caring for their loved one. Forty percent of family caregivers report feeling “down, depressed, or hopeless in the last two weeks,” according to a national survey of family caregivers.15 Nearly one-third of family caregivers whose responsibilities take 21 or more hours per week say that caregiving has made their health worse.16 The emotional and physical toll is not limited to those caring for older adults—caregiving can take a toll on those caring for loved ones of all ages.
Family caregiving is also a source of financial stress. Three of every four family caregivers use their own money to care for their loved ones, spending an average of nearly $7,000 in 2016 on caregiving costs.17 Caregivers aged 50+ who need to leave the labor force early to care for a parent forego more than $300,000 in lost wages, social security benefits, and pensions.18
All told, the economic value of family caregiving in the U.S. rivals the economy of a small country. In 2015, family caregivers provided 37 billion hours of care to adult care recipients, totaling about $470 billion in unpaid economic contributions.19 That amount is roughly equal to the gross domestic products of Belgium or Poland.20
2. The number of family caregivers is not keeping pace with demographic changes.
The declining supply of family caregivers, the aging of the population, and the increased responsibilities for those who do provide care will continue to create challenges into the future. In 2010, the ratio of potential caregivers (individuals aged 46-64, which are the most common caregiving ages) to aging seniors (aged 80+ who are most at risk for needing long-term services and supports) was about 7:1; that ratio is projected to be 4:1 by 2030 and 3:1 by 2050.21
Source: AARP Public Policy Institute, 2013.
3. Without family caregiving, the health of recipients would be worse and costs higher.
The declining supply of family caregivers will create challenges not only for care recipients and caregivers, but also for the entire health and long-term services and supports systems. Research has confirmed that family involvement in care avoids more costly health care services while leading to better health outcomes.22 These results come from a recent study of a Medicaid demonstration program that provided beneficiaries with an allowance to pay for care from a home care agency or from family and friends. Additional studies of broader populations of senior citizens have found that the availability of a family caregiver is associated with reduced frequency and duration of hospitalizations for older adults, reduced home health care utilization, and delayed entry into skilled nursing facilities.23
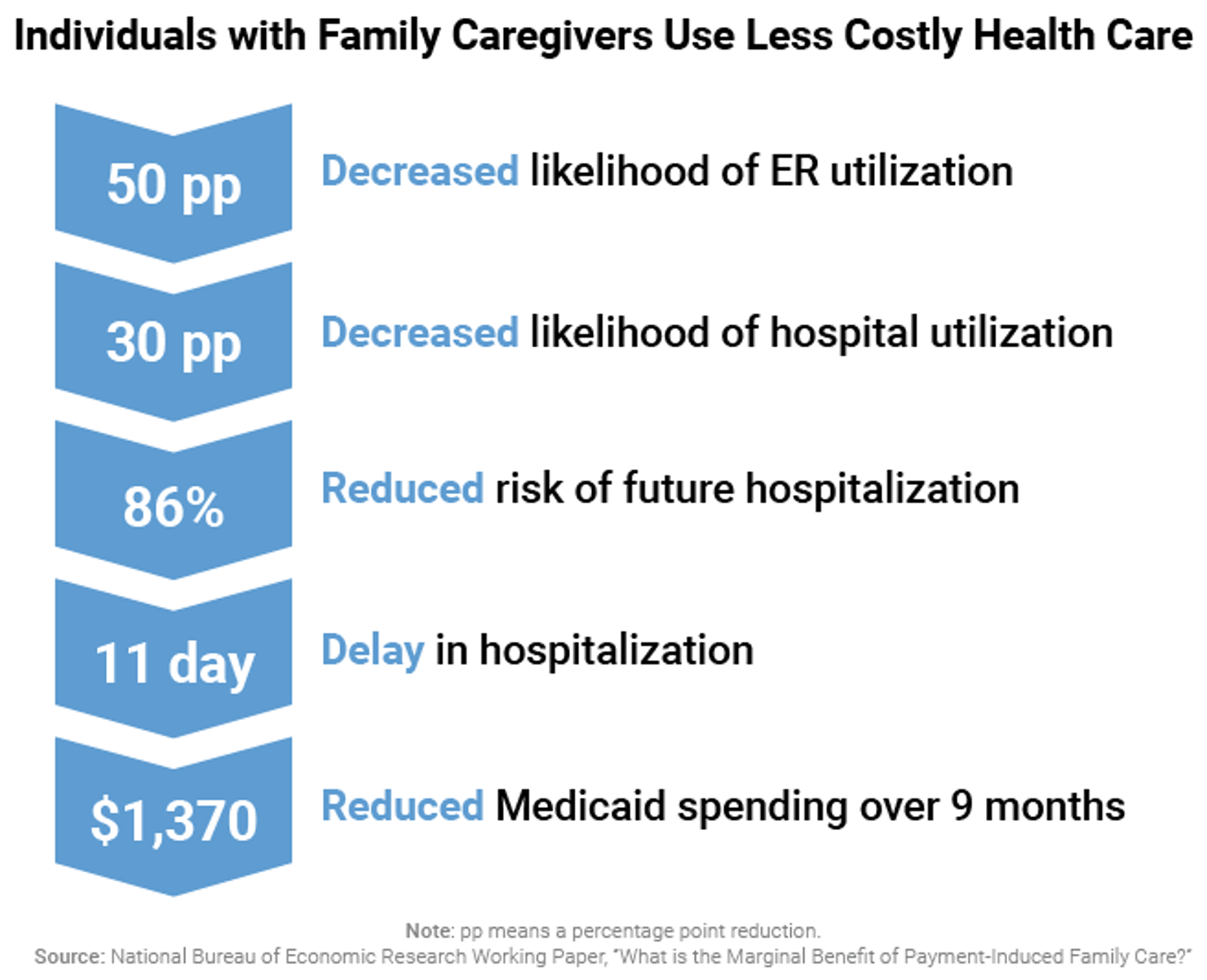
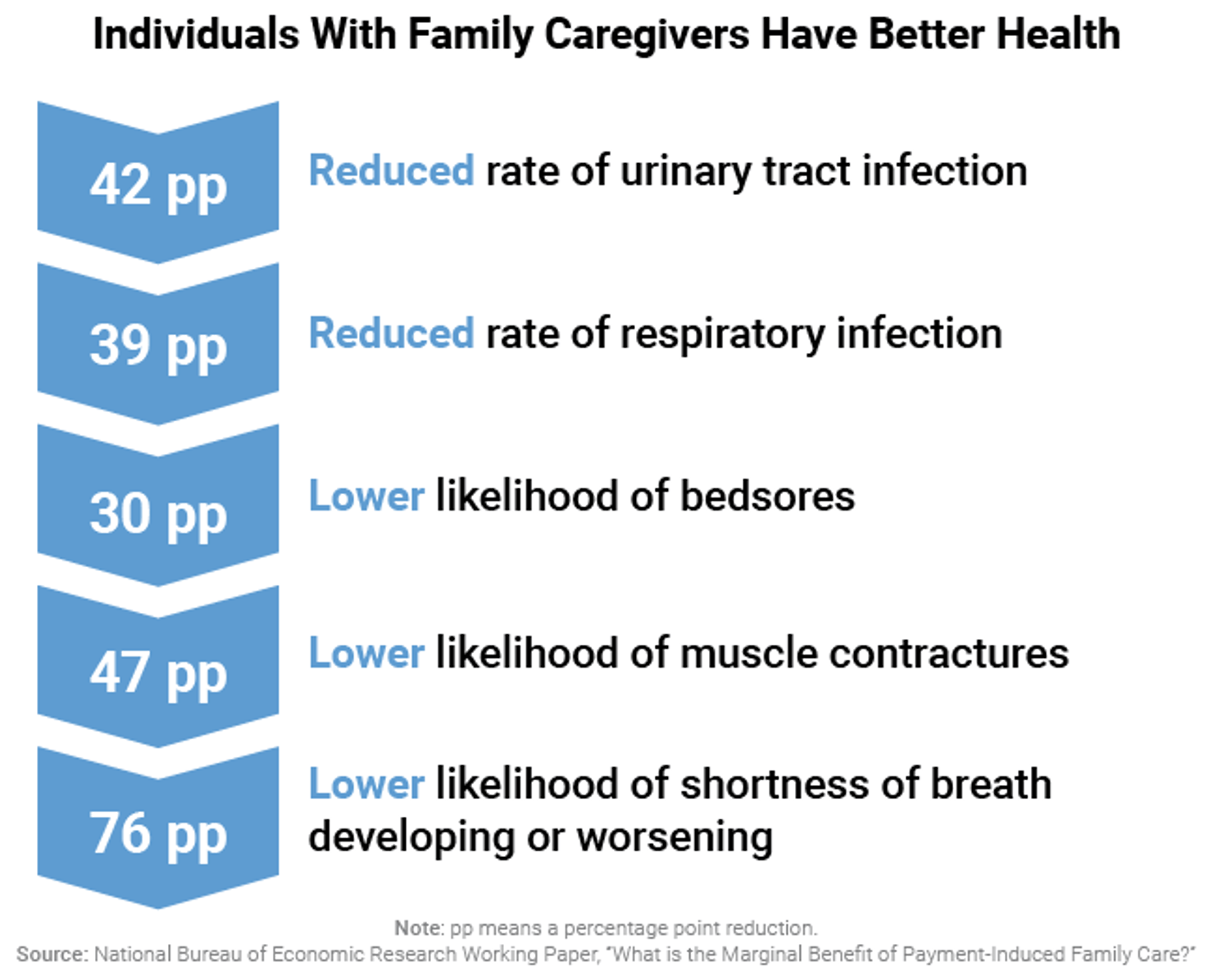
In short, family caregivers are critical in the effort to improve health care outcomes and lower costs in the U.S.
The Solution: A Strategy to Support Family Caregivers.
We need a strategy to support family caregivers. While family caregivers face a broad set of challenges, the responsibility for addressing them is diffuse. It is spread across social service organizations, health care and long-term services and supports organizations, community groups, employers, all levels of government, and others. For that reason, Senators Susan Collins (R-ME) and Tammy Baldwin (D-WI) and Representatives Gregg Harper (R-MS) and Kathy Castor (D-FL) have introduced the RAISE Family Caregivers Act.24 RAISE stands for Recognize, Assist, Include, Support, and Engage.
This bill would direct the Secretary of Health and Human Services to develop a strategy for supporting family caregivers. The strategy would identify actions that communities, providers, government, and others are taking and recommend actions they may take to recognize and support family caregivers. It would be updated biennially. It also calls for the creation of a Family Caregiving Advisory Council that would consist of representatives of key stakeholders to advise and work with the Secretary.
Significantly, the strategy would bring stakeholders together around supporting family caregivers. The bill would improve the collection and sharing of information, including information related to evidence-based or promising practices and innovative models regarding family caregiving. It would better coordinate, assess, and maximize the effectiveness of existing federal government activities to recognize and support family caregivers while avoiding duplicative efforts. The strategy and work around it could help inform and enable state and local efforts to support family caregivers as well.
That is why the RAISE Family Caregivers Act is the necessary next step in addressing this pressing national challenge.
Conclusion
Caring for a loved one with health or functional needs is just something we do. It is an act of love and basic humanity. As the stresses and challenges of family caregivers increase, and as most Americans will become either a family caregiver or care recipient at some point in their lives, the nation needs a strategy to help enable every community to support the family caregivers who are the frontline of care for the most vulnerable Americans. The RAISE Family Caregivers Act would provide that strategy.


