Memo Published June 25, 2015 · Updated June 25, 2015 · 16 minute read
Local Examples: Innovations in Drug Adherence
These abysmally low medication adherence
rates lead to more than 125,000 deaths and $290 billion in wasted spending in the United States every year. Among diabetes patients, for example, the cost of health care is twice as much for patients who are not taking the necessary medications. For all diseases, poor adherence may put patients in the hospital where care is more expensive. That costs the nation roughly $100 billion each year and contributes to one in ten hospital stays.
Patients, especially those who are not regularly taking their medications and those with chronic conditions where nonadherence is extremely costly, need drug therapy support services. Doctors, pharmacists, and health plans are working across the country to improve medication adherence using drug therapy management programs that target individual obstacles to adherence while determining who is accountable for improving patient outcomes and saving money.
For example:
Nationwide
Aetna Rx Healthy Outcomes
An option available to self-insured groups, Aetna’s Rx Healthy Outcomes program combines value-based insurance design with pharmacist outreach to increase medication adherence. Following a heart attack or cardiac procedure, such a receiving a stent, patients pay reduced copays for brand-name cardiac drugs and nothing for generic drugs. In addition, within a week of discharge, a pharmacist calls the patient to explain medications, reconcile new drugs with the patient’s previous regimen, answer questions, and connect the patient with their care providers if needed. Compared to a similar program that did not include pharmacist outreach, the Rx Health Outcomes program increased drug adherence rates by 4.4 percentage points for beta-blockers and 6.2 percentage points for statins. Patients also experienced a lower rate of stroke than those in the control group.
Express Scripts
Express Scripts, the largest pharmacy benefits managers in the United States, conducted a retrospective analysis of Medicare Part D beneficiary claims data to determine if whether beneficiaries received their prescriptions through home delivery or from a retail pharmacy had any impact on medication adherence. Eligible beneficiaries were followed for two years and were considered to be adherent if their proportion of days covered met or exceeded 80%. The analysis controlled for demographics, low-income subsidy status, disease burden, and prior adherence behavior. After analyzing more than 150,000 patients with diabetes, 615,000 patients with hypertension, and 358,000 patients with high cholesterol, researchers found that patients in all three disease categories who used home delivery were more likely to be adherent. Specifically, patients with diabetes were 1.25 times more likely, patients with hypertension were 1.29 times more likely, and patients with high cholesterol were 1.26 times more likely to be adherent.
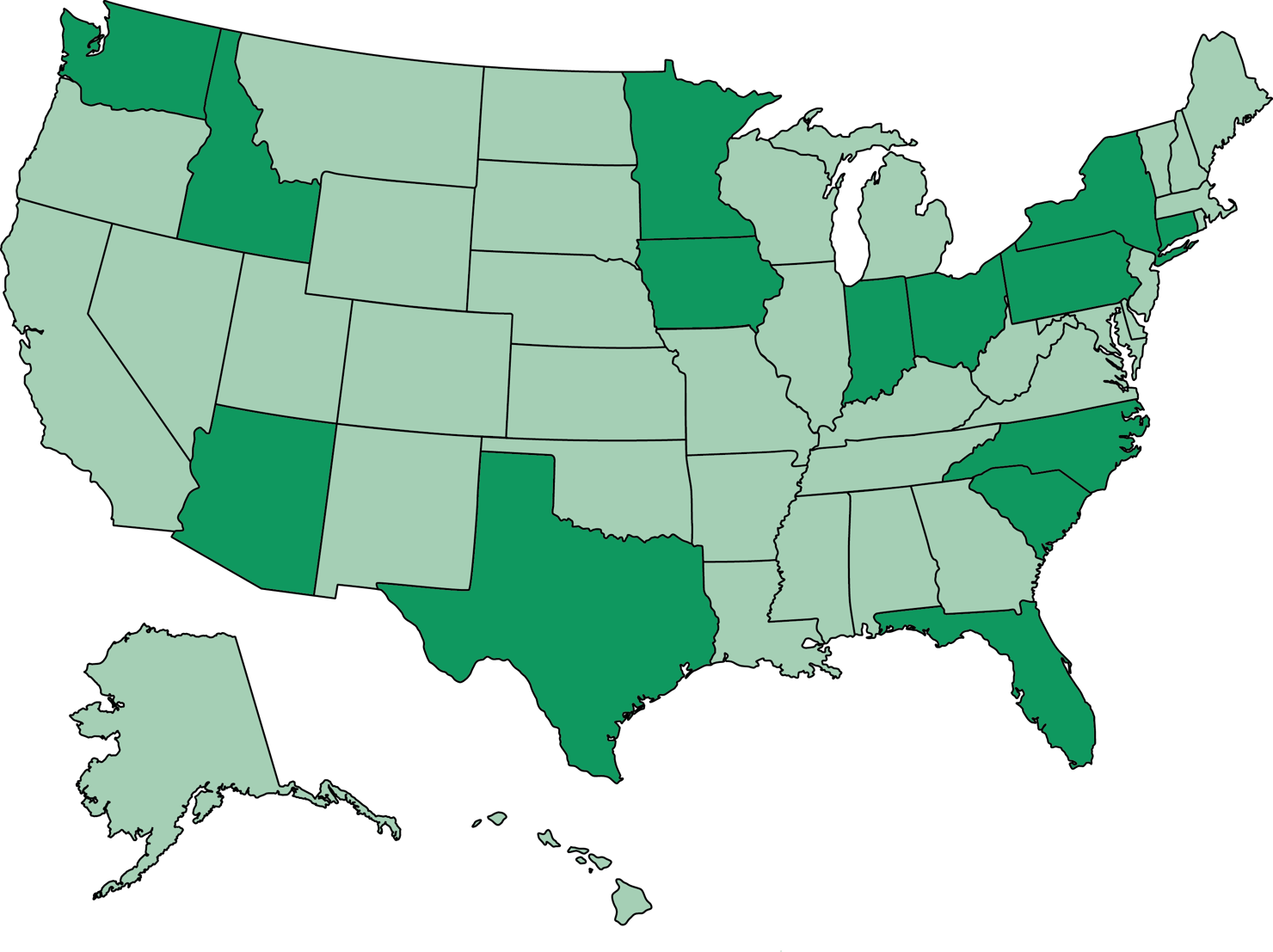
Project ImPACT: Hyperlipidemia, 12 States (Alabama, Delaware, Indiana, Iowa, Maine, Minnesota, North Carolina, Ohio, Texas, Virginia, Washington, Wisconsin)
Project ImPACT: Hyperlipidemia (Improving Persistence and Compliance with Therapy) is an initiative of the American Pharmacists Association Foundation. Hyperlipidemia, or high amounts of lipids (such as cholesterol or fat) in the blood is associated with increased coronary artery disease, which the leading cause of death in the United States. This project focused on evaluating the pharmacist’s role in promoting persistence (continuing to take a medication for the recommended duration) and compliance (taking medication according to prescribed timing and dose recommendations) of patients with high cholesterol. Twenty-six community pharmacies in 12 states participated in the study. Participating patients, either newly diagnosed with cholesterol issues or who were receiving lipid-lowering medications but were not well controlled, gave a very small blood sample at their initial visit to gather a fasting lipid profile. Patients then made follow-up visits every month for the first three months and quarterly thereafter. Pharmacists shared information with the patient and other members of their care team and involved patients in treatment plans and goal setting. Over the 24 months of the project, 93.6% of patients achieved medication persistence (meaning they continued their therapy for the duration), 90% achieved medication compliance (defined as missing less than five doses of medicine between each refill), and 62.5% achieved the National Cholesterol Education Program’s goal for lipid control.
Arizona
El Rio Community Health Center
El Rio is a federally qualified health center in Pima County, serving mostly patients with income at or below the poverty line. El Rio began collaborative drug therapy management in 2000, when onsite pharmacists first entered into collaborative practice agreements with community providers. About 800 patients receive collaborative drug therapy management services for diabetes and services are also available for patients with hypertension, hyperlipidemia, asthma, and other chronic conditions. The agreements permit pharmacists to assess patients, review all medications and adjust medications in certain drug classes, perform certain examinations, and review medications that require close monitoring, such as anticoagulation drugs. El Rio received payment for these services through Medicare Part D and as an accredited site for diabetes self-management training.
Connecticut
Department of Social Services
Using grant funding from the Centers for Medicare & Medicaid Services, the Department of Social Services conducted a demonstration project in which pharmacists provided medication therapy management services to Medicaid beneficiaries through in-person meetings in the offices of the patients’ primary care providers. Providers included four federally qualified health centers and one private practice. Patients brought with them all current medications, including prescriptions, nonprescription medication, supplements, and samples, and pharmacists also had access to patient’s electronic medical record and pharmacy claims data. Pharmacists were paid as independent contractors for their services and identified drug therapy problems, such as inappropriate medication, omission or duplication of medication, inappropriate dosage, and more, and resolved these issues. The pharmacists also worked with the patient’s health care providers to ensure drug therapy achieved treatment goals and to coordinate medication use across providers. Though the study involved a relative small sample (88 beneficiaries), the pharmacists identified 917 drug therapy problems, an average of 10.4 per patient, most of which were identified as preventable medication errors and required a pharmacists intervention. Nearly 80% of these problems were resolved, though 80% of resolved problems required the patient to meet separately with their primary care provider. Researchers estimate that an on annual basis, the interventions tested would yield $1,123 in medication savings per patient and $472 in medical and hospital savings, which are approximately 2.5 times the cost of the intervention.
Florida
Polk County
Polk County provides health benefits to more than 8,000 employees, dependents and retirees of county government through a self-insured plan. The County implemented a pharmacist intervention model to engaged patients with diabetes in managing their health and utilized an onsite clinical pharmacist. The pharmacist was an employee of CVS Caremark, the County’s pharmacy benefits manager. The program involved six half-hour counseling sessions and included copayment waivers for disease-related medications, supplies, and nonprescription products. The pharmacist coordinated with each patient’s primary care physician to address any gaps in care or contraindications. After one year, the percentage of patients with Hemoglobin A1c levels within therapeutic range increased from 55% to 72% with especially notable reductions in higher-risk patients. Blood pressure levels also decreased among participants, and claims analysis revealed a 30% reduction in hospital admissions and a 24% reduction in emergency room visits.
Idaho
Group Health Cooperative
In northern Idaho, Group Health Cooperative utilizes nurse case managers who work with patients to determine whether patients are managing their conditions, to help them understand their conditions, and to suggest tools, including financial assistance programs, that may help increase medication adherence. Group Health reports annual savings of more than $476 per participant.
Indiana
CVS Health
CVS Health’s Pharmacy Advisor program promotes discussions between diabetes patients and pharmacists, either in face-to-face counseling or on the phone. Pharmacists receive information from the Pharmacy Benefit Manager (PBM) so they can focus on potential problems with a patient’s adherence to medications and use of other therapies. The program proved effective at improving adherence rates and initiating recommendations for medication that had been missing from the patient’s treatment. The program is also cost-effective, with a return on investment of approximately $3 for every $1 spent.
Iowa
Osterhaus Pharmacy
About 60% of the patients served by Osterhaus Pharmacy, an independent community pharmacy in Maquoketa, have diabetes, hypertension, and/or hyperlipidemia—chronic diseases that may be better managed with collaborative care. The pharmacy began implementing elements of collaborative drug therapy management in 2000 and, today, provide medication therapy management services through information agreements with two local clinics. Osterhaus Pharmacy also provides immunizations to patients through an agreement with one of these clinics.
Minnesota
HealthPartners Medical Group
Pharmacists at HealthPartners Medical Group offer members an opportunity to participate in medication therapy management (MTM) programs, which are programs aimed at assisting patients with issues like medication adherence. In this program, health care providers can easily refer patients to pharmacists so they can provide an explanation for all the medications and assist patients with their questions and concerns. One trial of 450 adults found that the proportion of patients who reduced their blood pressure to recommended levels was much higher amongst HealthPartners patients receiving MTM services. One study found that the overall cost of care was 19% lower in MTM patients than patients without MTM benefits.
BlueCross BlueShield
As part of a study, BlueCross BlueShield identified nearly 300 members in Minnesota who had at least one of 12 different chronic conditions and were receiving care at one of six Fairview Health Services clinics in which medication therapy management services were provided. Overall, the patients studied averaged 6.4 medical conditions and used 7.9 different drug therapies. Pharmacists collaborated with primary care physicians to provide medication management services and identified a range of drug therapy problems, including the need for additional medications, the use of unnecessary medications, wrong dosage levels, and more. Pharmacists identified and resolved an average of 2.2 problems per patient, and 78% of problems were resolved without physician involvement. Hypertension goals were achieved in 71% of the study population (compared to 59% in a comparison group), and cholesterol goals were achieved in 52% of the study group (compared to 30% in the comparison group). Notably, during the year in which patients received medication therapy management, total health care costs were 31.5% lower than for the comparison group. While medication costs actually rose nearly 20%, facility and professional cost decreases more than offset these costs.
New York
Capital District Physicians’ Health Plan
The Capital District Physicians’ Health Plan uses a medical home model, called the Enhanced Primary Care Initiative, where pharmacists visit care teams and meet with patients about their medication regimen. Pharmacists in the pharmacy medical home model also help patients understand their medications, address any concerns, and help simplify their regimens. Additionally, pharmacists visit physician offices and provide physicians with recommendations based on their comprehensive medication reviews of patient records. As a result of this program, the overall hospital admission rate for Part D members enrolled in the program was 19% lower when compared with nonparticipants. Additionally, the readmission rate of the patients enrolled in the program was 27% lower than nonparticipants.
Collaborative Drug Therapy Management Pilot Project
In 2011, New York passed legislation permitting pharmacists practicing in the state’s teaching hospitals to participate in collaborative drug therapy management (CDTM). The law sunsets on September 15, 2015, though the legislature is considering legislation to expand the law and make it permanent. Several participating teaching hospitals provided CDTM outcomes data which was used to develop a report to the state legislature. For example, patients prescribed oral anticoagulants to treat and prevent blood clots must be closely managed to guard against bleeding risks. A test called the international normalized ratio (INR) provides a measure of the percent INR Time-in-Range. Patients managed by pharmacists achieved higher Time-in-Range (71.4-84.6%) than expected with usual care (51-76%). Similarly, the percentage of patients with diabetes managed by pharmacists who had Hemoglobin A1c levels within the therapeutic target increased by 22%. Thirty-day heart failure readmission rates dropped by at least 62% and 90-day readmission rates fell between 6-15%.
North Carolina
The Ashville Project
The Ashville Project begin in 1997, providing education and counseling to city employees, retirees, and dependents with chronic diseases. The program involves pharmacist-directed medication therapy management services and has expanded to include several employers in the city. A study focused on improving hypertension and dyslipidemia outcomes involved employers who already offered medication therapy management programs to employees with diabetes or asthma. Patients agreed to complete education regarding cardiovascular risk reduction and to meet with a care manager or coach as often as once per month on a long-term basis, and received significantly reduced copayments on blood pressure and cholesterol medication. The study found significant improvements in the percentage of patients who met their blood pressure goals and a 53% reduction in the risk of a cardiovascular event. Hospitalizations and emergency room visits also decreased by 54%. While, average cardiovascular-related drug costs increased by 290%, or $559 per person per year, these cost were more than offset by a drop in average health plan expenditures for cardiovascular-related medical costs of 46.5%, a savings of $628 per person per year.
Ohio
OutcomesMTM, Medicaid Program
OutcomesMTM partnered with Caresource, one of the country’s largest Medicaid managed healthcare plans, to implement and oversee a comprehensive MTM offering for the Ohio Medicaid population. OutcomesMTM designs, delivers, and administers MTM programs. Since 2012, the program has seen a drug product cost savings of $1.30 on every $1 spent on MTM services. These findings show that savings can be achieved on both the drug and medical spending.
Pennsylvania
Geisinger Health System
Geisinger’s collaborative practice model refers patients at high risk of hospital admission or readmission to a pharmacist specializing in disease management. These specially trained pharmacist conduct a series of face-to-face and phone consultations with patients over a period of weeks to month, depending on patients’ needs. Pharmacists begin by asking patients what their goals are and linking medication adherence to the achievement of those goals, ensuring drug regimens align with patient preferences. Pharmacists continue this intensive intervention until the patient reached recommended clinical targets, and remain available if a patient’s condition later worsens. Between December 2010 and March 2012, 3,000 patients received these medication management services. Eighty-four percent of patients reduced their Hemoglobin A1c levels, with 64% reaching their clinical target, 72% reached cholesterol target levels, and 70% reached their blood pressure target. In addition, just 8% of patients treated with anticoagulant medication and receiving medication management services experienced bleeding, compared to 17% of similar patients not participating in the program.
PerformRx Drug Therapy Management
PerformRx, a pharmacy benefits manager and part of the AmeriHealth Caritas Family of Companies, combines drug therapy management software with pharmacist care coordination to reduce hospital admissions and total costs for Medicaid managed care members with diabetes taking 15 or more medications. PerformRx’s software alerts pharmacists regarding unfilled prescriptions, duplicative or dangerous drug combinations, dosing errors, and other potentially adverse events. In response to an alert from the software, pharmacists may reach out to the health plan’s care managers, who assess the reasons for the patient’s prescription non-adherence and connect patients with services or strategies to increase compliance. In some instances, pharmacists may contact the patient’s prescribers directly to address certain issues, such as dangerous drug interactions or duplicative treatment. Hospital admissions for members who received these services declined by 10.4%, compared to the control group’s increase in admissions of 66%. Pharmacy costs for the intervention group increased half as much, for Keystone First members, and about one-third as much, for AmeriHealth Caritas Pennsylvania members, and total medical and pharmacy costs were about 50% lower for both plans compared to the control group.
South Carolina
BlueCross BlueShield of South Carolina
To improve medication adherence among members with cardiovascular disease and/or diabetes, BlueCross BlueShield of South Carolina implemented a behavioral intervention, called the Longitudinal Adherence Treatment Evaluation, as part of a broader care management strategy. The health plan analyzed pharmacy claims data to identify patients prescribed certain medications for cardiovascular disease or diabetes who were 60 or more days overdue for a refill. Care managers, who received training on techniques for medication behavior change, addressed the overdue refills during their next patient contact. Care managers were trained to address common barriers and available resources, such as side effect managements, mail order medications, financial assistance programs, and medication organizers and reminders. Patients who received this intervention were much more likely to resume taking their medication compared to a control group (59.3% versus 42.1%) and took much less time to resume drug therapy (59.5 days compared to 107.4 days).
Texas
KelseyCare Advantage
KelseyCare Advantage is a Medicare Advantage plan sponsored by the insurance arm of the Kelsey-Seybold Clinic, an integrated payer-provided in the Houston area. The plan has used collaborative practice agreements since 2004 to facilitate close cooperation between pharmacists in physicians, and these agreements were expanded in 2008 to cover additional medications. One program targets patients with diabetes, high cholesterol, and hypertension. When these patients do not fill or refill prescriptions within a week of the prescribing or refill date, pharmacy technicians reach out to determine why. These technicians help patients who simply need reminders with strategies like pill boxes, smartphone apps, or automated refill services. If patients need assistance with pay for medications, are experiencing side effects, or face other issues, pharmacists connect with other members of the care team to meet these needs. From 2012-2013, the proportion of members taking diabetes medications as recommended rose from 76% to 83%, statin adherence for high cholesterol grew from 71% to 82%, and adherence to high blood pressure medications increased from 77% to 86%.
Washington
Group Health Cooperative
Group Health Cooperative’s patient-centered medical home (PCMH) model utilizes medication therapy management to increase drug adherence through a number of different pharmacist-led strategies. First, pharmacists engage new patients at any of Group Health’s PCMH clinics in a medical onboarding process, which occurs before the patient’s appointment with a primary care physician and involves review of health conditions and prescriptions to highlight safety issues and opportunities to provide evidence-based care, simplify drug regimens, improve health outcomes, and save money. In addition, Group Health’s collaborative practice model, certain Group Health pharmacists can prescribe and change certain medications for patients with chronic, complex health conditions. Pharmacists work with patients for four to five months, conducting a comprehensive medication review, working with the care team to identify treatment and outcomes goals, and evaluating how well drug regimens are working to achieve those goals. Finally, pharmacists also help patients discharged from the hospital with chronic conditions safely transition to outpatient care. Pharmacists compare discharge summaries with the patient’s electronic health record medication lists, identifying potential problems and coordinating with the care team to address any discrepancies. Pharmacists contact patients 3-7 days after discharge to review each medication’s purpose, does, and other instructions and to answer any questions. A study of nearly 500 patients found hospital readmission rates at seven and 14 days after discharge were much lower for participants receiving these services. This translates into a savings of approximately $35,000 per 100 patients, or $1.5 million per year.
