Report Published September 29, 2015 · Updated September 29, 2015 · 23 minute read
A Better End of Life
David Kendall & Elizabeth Quill

Nancy is 87 years old, lives in Milwaukee, WI, and is dying of advanced stage cervical cancer.1 Her physician presents an aggressive treatment plan, but Nancy is not sure how she wants to proceed. She is overwhelmed and doesn’t know whether she should aggressively fight during what could be the last few months of her life, or if she should focus on spending her last few months comfortably. On top of that, she hasn’t discussed an advance care plan with her physician or specified her goals and preferences for medical treatment in an advance directive.
If Nancy had lived in La Crosse, Wisconsin, she wouldn’t have been in this predicament. Approximately 96% of people who pass on in La Crosse have an advance directive outlining their wishes because Gundersen Lutheran Medical System sought to make discussing end of life wishes a comfortable conversation. Gundersen even works with medical providers within community churches in LaCrosse to better engage individuals in comprehensive end of life planning before they face life-threatening situations.2
By changing when people start to express their health care preferences and how individuals and health care professionals treat conversations about care at the end of life, people are more likely to get the care they actually want if they cannot speak for themselves. Moreover, by simply increasing the likelihood that people will use advance directives that are accessible when and where needed, the federal government could save as much as $15.2 billion over 10 years.
This idea brief is one of a series of Third Way proposals that cuts waste in health care by removing obstacles to quality patient care. This approach directly improves the patient experience—when patients stay healthy, or get better quicker, they need less care. Our proposals come from innovative ideas pioneered by health care professionals and organizations, and show how to scale successful pilots from red and blue states. Together, they make cutting waste a policy agenda instead of a mere slogan.
What is Stopping Patients from Getting Quality Care?
Most older Americans want to live their final days at home.3 Despite this, they usually die in a hospital or nursing home, with only 24% able to die in their homes.4 Why does this happen? Of course, circumstances can get in the way of a person’s goals and preferences for medical treatment if and when that person becomes a patient. But, more often, doctors and patients have not discussed and documented what a particular patient wants if he or she cannot communicate. Thus, people end up receiving the default standard of care where doctors do everything possible to extend life.5 A recent Institute of Medicine (IOM) report noted:
“Most people envision their own death as a peaceful and an ideally rapid transition. But with the exception of accidents or trauma or of a few illnesses that almost invariably result in death weeks or months after diagnosis, death comes at the end of a chronic illness or the frailty accompanying old age.”6
Unless people work with their doctor on alternatives, they will receive all the care possible that keeps them alive.7 NPR’s Linda Poon described this as “needlessly painful experiences suffered by many patients.”8 In fact, this treatment is often adverse to what individuals themselves desire.9 In one study, 71% of respondents favored enhancing quality of life over extending life through all possible interventions.10
People need help understanding how to handle the choices that may arise with their health care. This includes discussions with health care providers and family members. Individuals need to have conversations with providers about the care they want in emergencies and—especially at the end of life—if they cannot speak for themselves. They need to discuss their goals and preferences for medical treatment with their family and surrogates—and help their family members do the same.11 They also need to name a surrogate decision-maker with whom they have discussed goals and preferences at length and who will make choices consistent with those wishes.
Furthermore, people need to document their wishes and make those plans easily accessible so that family members, caregivers and medical treatment providers can follow them when necessary. Studies show that only 18-36% of American adults have completed an advance directive (AD)—written instructions that allow individuals to make decisions about their care ahead of time in case they become incapable of participating in these decisions later—and that less than 2% of individuals who have ADs have access to them when needed.12
A comprehensive advance directive addresses specific situations, like the use of feeding tubes, and provides physicians and family members with guidelines to make decisions for an individual if he or she ever becomes a patient and cannot communicate with health care providers.13 Depending on the state, ADs are also known by names like “living wills,” “medical powers of attorney,” and “personal directives.” For an individual’s convenience, these various legal documents can be combined into a single form that can be digital or paper-based. Physician Orders for Life-Sustaining Treatment (POLST) forms are another tool that turns a patient’s preferences into standing orders from a physician. Such orders are particularly important when patients get transferred to multiple care settings and receive care from providers who are unlikely to know the patient’s preferences.
Without an AD, an individual is more likely to receive unwanted, aggressive care, and physicians and family members are less likely to follow that person’s goals and preferences for medical treatment. ADs work best when:
- The person completing them understands the terms of the AD and the implications of his or her decisions;
- The person’s family understands the person’s wishes as expressed in the AD;
- The physician can easily access the AD; and
- The AD is revised as necessary by the person throughout his or her life.14
ADs can also remove any doubts that a person wants aggressive treatment if that is their wish. Contrary to some misperceptions, ADs do not limit care; they let patients express their preferences about their care when they cannot speak for themselves.15
The ideal use of ADs is complicated, however, by behavioral traits—essentially cognitive biases—that affect a person’s decision-making. For example, it is difficult for people to predict their future preferences without heavily relying on their current preferences. Making difficult choices for future scenarios is challenging, notwithstanding accounting for how one might die. Behavioral scientists call this present bias, which explains why what you want now doesn’t always align with what you may want in the future, and how it’s difficult to set aside desires in the present when making a decision that will promote one’s goals in the future. Studies show that people often make choices that their future self would not have made.16 Overcoming present bias in decisions about end of life care can start with creating an AD early in life much the way like organ donation already works. Updating the AD as one grows older and gets more experience with end of life issues is then easier for individuals, loved ones, and providers.
Other barriers to the effective use of ADs are entrenched in current attitudes and practices surrounding their use. Rather than using them as a tool to develop and record individual preferences about care, families and health care providers do not turn to ADs until a person is incapacitated or “absolutely, hopelessly ill” before translating his or her goals and preferences for medical treatment into care plans, as noted in a 2008 report to Congress prepared by the Department of Health and Human Services.17 Furthermore, frequent transfers of patients across care settings (like hospitals to nursing homes) increase the risk that ADs completed in one care setting will not be transferred to a new setting with the patient. Finally, the fact that ADs can be legalistic, static documents with detailed signature and witnessing requirements creates obstacles to their completion and on-demand use.
Where are Innovations Happening?
Innovative efforts throughout the nation have increased awareness and use of ADs, while also making them more accessible. For example, some states have created online registries where people can file their advance directives, and physicians can access online databases. Louisiana created the first registry in 1991 which allows physicians and health care facilities to request access to a patient’s AD.18 In other states, individuals can either upload their AD into a registry or register the location of their AD.19 The Caring Connections website provides simple instructions for creating an AD in each state along with a template.20 Private companies like MyDirectives (a free service) and DocuBank (another service that charges consumers an annual fee) allow consumers to access and share their ADs online.21 Digital ADs like MyDirectives have made it easier for people to create, store, update, and instantly share high-quality care plans.
Across the United States, health information exchanges (HIEs) are also using technology and data transfer standards adopted worldwide to connect care plan registries and improve accessibility of ADs. For example, the Chesapeake Regional Information System for our Patients (CRISP), a regional HIE serving Maryland and the District of Columbia, is working with MyDirectives to improve the accessibility of high-quality advance care plans to physicians in the region.22
Since 2007, the National Healthcare Decisions Day has spread awareness about the importance of ADs. After that event in 2013, the West Virginia Center for End-of-Life Care, which houses West Virginia’s online registry, saw a 35% increase in the filing of ADs.23
ADs are also becoming apps. The American Bar Association has released a smartphone application called “My Health Care Wishes” that allows patients to store their ADs or family members’ ADs and share them when necessary.24 MyDirectives has a mobile application for Apple iPhones and iPads that lets consumers use video and audio recording, electronic signatures (with location, date, and time stamps to ensure authenticity), and email and texting to record and share their goals and preferences for medical treatment.25 These easily accessible and navigable digital tools are increasingly popular with younger consumers.
Hospitals are also seeing lower spending as a result of AD efforts. Specifically, advance directives that limit end of life treatment have been shown to lower spending in hospitals with high levels of spending in patients’ final days.26 For example, in La Crosse, Wisconsin, Gundersen Lutheran Health System has successfully expanded the use of advance medical directives through a community-wide advance care planning program. The program incorporates disease specific planning and a medical home for patients’ last two years of life that includes primary care, hospice, social services, and home health.27 The program is integrated into Gundersen Lutheran’s routine primary care visits, as well as non-clinical, community settings via trained advance care planning “facilitators,” so that advance directives are discussed, considered, and created well in advance of end of life care.28 The advance directives are maintained in Gundersen Lutheran’s electronic medical records.
Since its creation in 1986, the program has been enormously successful at increasing both the existence and accessibility of advance care plans in La Crosse. In 2010, among adult La Crosse residents who died over a seven-month period, 96% had some form of advance care plan, 99% of those plans were available in patients’ medical records, and treatment was consistent with the advance directives in 99% of the cases.29 Gundersen’s programs are intensive—with high upfront costs and daily challenges like getting full participation.30 Nonetheless, it has cut the cost of care in the last two years of life by nearly half, from a national average of $79,337 to $48,771 in their area.31
In a separate effort, clinical leaders at Care Support of America of the University at Albany (a part of the State University of New York) and Kaiser Permanente collaborated to develop the Advanced Illness Coordinated Care Program—a pilot program that experienced success with coordinated palliative care.32 The program targeted patients with advanced illness to “better understand their illnesses, communicate with providers, and reduce barriers to palliative care when appropriate.”33 This program involved social workers addressing advance directives with patients. Under this program, patients were 2.23 times more likely to complete an AD.34
And in Chicago, a group from Rush University Medical Center is providing basic palliative care skills to local physicians and advanced practice nurses by pairing them with “mentors, hosting conferences, and offering online learning.”35 The goal is for those trained to create a network of providers who can learn from each other and also train other providers on how to communicate well with patients and families about advance care planning.36
The Coalition to Transform Advanced Care (C-TAC) and the AHIP Foundation have documented best practices for advanced illness care as part of their collaboration, the Advanced Care Project.37 For example, they have shown how several health plans have worked with patients living with a serious illness care as well as their physicians to offer management services that ensure patients get the care they really want. Some of these patient-centered programs have found that providing compassionate care to patients in accordance with their wishes goes hand-in-hand with reducing costs due to the patient foregoing unwanted interventions. A program created by Aetna and led by physicians produced the same or better quality of life for the patient while also reducing costs by as much as $12,000 per member for each year.38 Another health plan, Humana is working to bring advance directives directly to its members.39 Overall, the project aims to bring providers together and identify ways to “sustain the delivery of quality, evidence-based person-centered care for those with advanced illnesses.”40
How Can We Bring Solutions to Scale?
Every American should know they can express their preferences for medical treatment—and that medical professionals and family members will have access to and respect their wishes if he or she cannot communicate. All consumers aged 18 and over need help understanding the choices available to them and the implications of their decisions. They also need help expressing and recording their goals and preferences for emergency, critical, and end of life medical treatments, and doctors need to adjust their medical practices to learn and act on a person’s preferences when and if that person ever becomes a patient.
Public policy should provide increasing levels of support for promoting advance care planning for all Americans—not just those who are older, frail, or chronically or terminally ill. This should start with normalized education and general encouragement for all adults, include comprehensive counseling for patients with advanced illness, and progress to specific rewards for Medicare beneficiaries. This should happen in three ways:
- Combine existing programs with new technology to make high-quality advance directives available and accessible for all adults.
- Provide in-person counseling to patients with advanced illness and their families, when warranted.
- Encourage Medicare beneficiaries to have comprehensive, digital advance care plans that include ADs, and make it easier for doctors to respect them with increased quality, portability, and accessibility.
First, use technology to make high-quality advance care plans available and accessible for all adults.
The first step to ensure that a person’s goals and preferences for medical treatment are followed is to create a care plan with a high-quality AD. This should cover not only end of life care, but also emergency care and critical care. Both the Department of Health and Human Services (HHS) and the Institute of Medicine have called on the health care industry to use technology to ensure that ADs are accessible to all adults and easily available to their caregivers and medical professionals. Today, ADs too often cover only general questions about patient preferences and are not specific enough to help caregivers and providers make specific decisions. ADs are also too often found only on paper, hidden away in filing cabinets or safety deposit boxes. Policy changes in four areas can help solve these problems:
- The Patient Self-Determination Act of 1990. This law currently requires many health care providers (like hospitals and nursing homes) to provide basic information to patients on advance care planning. The law, as well as the federal regulations adopted under it, should be amended to require information on electronic ADs. Having a high-quality AD available online would give consumers more assurance that their wishes would be accessible and increase the likelihood that others would follow it. Congress should also consider tightening up the enforcement of the act to address gaps and challenges identified in a recent General Accountability Office report.41
- Standards for lawyers who create ADs. Some people complete a paper-based advance directive when they create a will with their attorney. The American Bar Association (ABA) has been a long-time proponent of advance care planning and ADs42 and, as mentioned above in this idea brief, has released a smartphone application to help consumers store and share their ADs. State legislators should work with the ABA and amend their Rules of Professional Conduct to state that lawyers must strongly encourage their clients to have an electronic copy of their AD either uploaded on a state registry or a private registry service so they are always available anywhere in the world. These registries allow patients to register their AD information either by uploading a PDF of their AD or by providing a link to an existing AD. The optimal digital access is one that seamlessly integrates into health information exchanges and electronic health records platforms, significantly increasing the likelihood that the current version of a person’s AD will be located and retrieved when needed. Consumers usually complete an agreement that gives the registry permission to send copies of their AD to health care providers, by paper or digitally, which a law office could help facilitate if necessary.
- Standards for electronic health records in patient-centered medical homes. Only 25% of physicians know of their patient’s existing AD once a patient has created one.43 Ideally, all electronic health records platforms would be required to have the ability to proactively query a registry, an HIE, or a service like MyDirectives in order to locate a person’s care plan and AD—and to be able to embed a link to the person’s AD in the electronic medical record. In fact, MyDirectives is the first advance directive platform to receive meaningful use certification from HHS.44 Advancing ADs could happen quickly through medical homes, which is a team of health professionals led by a physician who watches over an individual’s health using modern communications and information technology.45 The National Committee on Quality Assurance, which sets standards for quality measurement for medical homes, recommends that medical homes have an AD link in their EHRs.46 Many private health plans incorporate similar standards into their own medical home guidelines, and federal standards for medical homes like those from the National Committee for Quality Assurance should make an AD link a required practice.47
- Continuing medical education. Primary care physicians can play an important role in helping patients to have a conversation about the kind of care they want if they ever find themselves unable to effectively communicate with caregivers or physicians. Simply handing out information to patients about emergency care plans, Ads, and end of life care is not sufficient. Patients who discussed advance care planning preferences with families and physicians report having less fear and anxiety, felt they had more power over their care, and felt better understood by their physicians and families.48 However, physicians find that starting conversations about end of life is difficult. Therefore, both patients and physicians tend to avoid these conversations.49 End of life care education in both medical schools and Continuing Medical Education (CME) courses is one way to help physicians become comfortable having these consultations.50 Medical and nursing schools should follow the standard set by the University of Minnesota Medical School and require their students to lead by example and create digital ADs. Congress (which provides funding for medical education) and states (which oversee medical licensure requirements that includes CME) should ensure that physician education includes training on how to discuss and develop advance care plans including ADs with patients.
Second, provide in-person counseling to patients with advanced illness and their families, when warranted.
Doctors, nurses, social workers, and other medical treatment providers must be properly reimbursed for having end of life conversations. Furthermore, quality measures must be implemented that aim to measure effectiveness of these conversations. Both of these are necessary steps that would ensure valuable conversations take place at a more substantive level than just a quick checklist. The verification or creation of an AD as part of these conversations is a critical element in order to record a person’s preferences for all types of care—ranging from emergency care, to critical care, to end of life care.
In June 2015, Senators Mark Warner (D-VA) and Johnny Isakson (R-GA) re-introduced the Care Planning Act, which would create a Medicare and Medicaid benefit for end of life consultations among other provisions.51 It would codify the proposed regulation by the Centers for Medicare and Medicaid Services to provide Medicare coverage for such consultants.52 Specifically, this legislation would work to reimburse health care professionals for having a discussion about a patient’s goals and options resulting in a written plan reflecting the patient’s preferences.53 In order to ensure that these conversations are meaningful, it is also necessary to implement quality measures that work concurrently with the reimbursement reforms. A comprehensive study of end of life quality measures has identified a significant gap in quality measurement efforts for advance care planning.54 Representative Earl Blumenauer (D-OR) has previously introduced similar legislation called the Personalize Your Care Act.
The Care Planning Act would also require HHS to develop quality measures on end of life care. The measures would include how well providers took account of each person’s goals, values, and preferences. Specifically, providers should be able to explain how a care plan reflects the way a patient wants to live, and then the quality measure can assess how much the care is consistent with a person’s goals, values, and preferences across all care settings.
Coordinated palliative care, which works to improve quality of life for very sick patients, can also enhance patient well-being and reduce costs.55 It is critical for these patients to have conversations about end of life if they have not already done so. Building advance care planning initiatives into coordinated care models will help these patients receive the care they intend. Existing coordinated care models have used social workers as counselors to address end of life and ADs with patients multiple times and as their conditions progressed.56 These models have proven to expedite the process of creating an AD.57 Other models use registered nurse case managers to determine whether patients have an existing AD and, if not, educate patients on their potential decisions and options.58
Third, encourage Medicare beneficiaries to have comprehensive, digital advance care plans that include ADs, and make it easier for doctors to respect them with increased quality, portability, and accessibility.
Advance care planning becomes increasingly important as a person grows older and faces a higher risk of life-threatening conditions. Encouraging Medicare beneficiaries to complete ADs with a simple reward can get more people engaged. Medicare should also require providers to report on their success in getting ADs included in electronic health records so an AD will be easily accessible and available when it is needed. State and federal legislators can ensure that consumers’ care plans and ADs will be respected and followed by standardizing the law relating to ADs and focusing on substance over form. Policy changes include:
- Encouraging beneficiaries. In 2014, Senators Tom Coburn (R-OK) and Chris Coons (D-DE) introduced the Medicare Choices Empowerment and Protection Act, which provides Medicare beneficiaries a one-time reward for establishing an AD created by outside organizations, with a larger reward being made for the creation of an electronic AD.59 CMS would not have a copy of the AD but would instead track the organization that maintains the beneficiary’s AD.60
- Reporting Success on ADs in Electronic Health Records. Building off the accessibility recommendations above, Medicare providers can also be required to report on their inclusion of ADs in electronic health records—an important step in making sure that ADs are easily accessible when they are needed. Currently, recording the existence of ADs in EHRs is listed as a Stage 1 and Stage 2 Menu Objective for the Centers for Medicare and Medicaid Services’ (CMS) EHR Incentive Program.61 Under this objective, the goal is to have more than 50% of patients 65 or older and are admitted to the hospital receive an AD status recorded in their EHR.62 However, despite the repeated recommendations of the HIT Policy Committee, the American Medical Association, the Joint Commission, and the National Quality Form, CMS has thus far chosen not to require either the recording of such AD status in an EHR or the embedding of a link in an EHR to any such AD. Strengthening the meaningful use regulations would require that the EHR have access to the AD either by storing a PDF of the AD or by embedding a link to an electronic AD in the EHR. Additionally, providers should report how many patients have ADs listed in their EHRs, how often such ADs are accessed and reviewed, and whether such ADs have been followed in a health care crisis.
- Standardizing state laws relating to ADs. HHS, the IOM, and the ABA have all reported that disparate state law requirements with respect to the content and signature/witness requirements of ADs, as well as a focus on legalistic, paper forms with little instruction or explanation to consumers, have acted as significant barriers to the adoption and effective use of ADs. Representative Earl Blumenauer’s Personalize Your Care Act would require, among other things, that in the absence of a validly executed AD, any “authentic expression of a person’s wishes with respect to health care be honored.”63 Federal and state legislators need to adopt measures to ensure that any expression by an individual of his or her goals and preferences for medical treatment in a health care crisis will be respected and not discarded simply because the person may not have used a particular form that he or she would likely not have been able to understand anyway.
Potential Savings
Savings to the Medicare program could accrue through adoption of policies that respect and enforce consumers’ choices with respect to the medical treatments they want (or do not want) to receive if they cannot communicate with their caregivers and physicians. When high-quality ADs are used in the Medicare population, it has been shown to reduce costs in high-spending regions.64 For example, a study found that Medicare patients in high-spending regions who chose a treatment-limiting AD cost an average of $33,933 in contrast to Medicare patients without an AD who cost an average of $39,518. Using rewards for Medicare patients will increase the number of Medicare patients with an AD. Digital care plans that include high-quality, actionable ADs along with web-based links to those plans in electronic health records and personal devices will increase access to them and increase adherence to a person’s wishes. Palliative care models have experienced significant savings at Gundersen Lutheran, where the program has resulted in an average of 13.55 hospital days per patient and $37,289 in total Medicare expenditures, compared to the national average of 23.6 days of hospitalization and $55,838 in total program costs.65
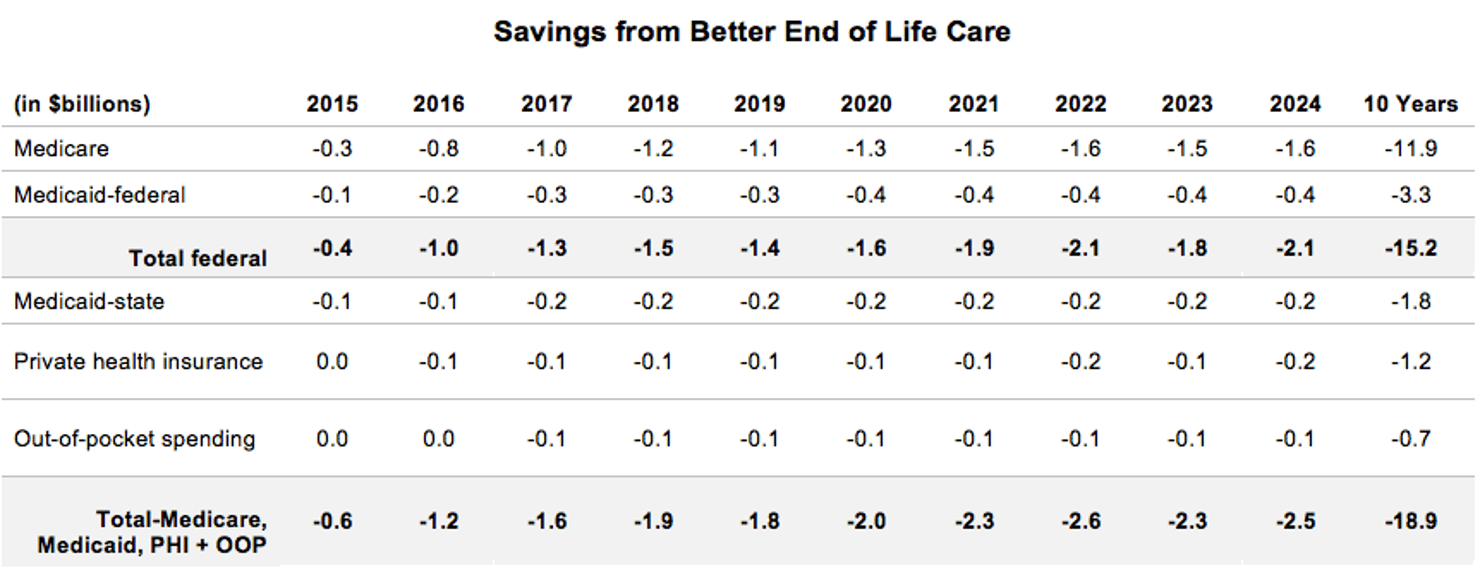
As shown in the chart below, Third Way estimates that these programs would decrease federal spending by $15.2 billion over the 2015-2024 federal budget window.66 It would decrease states’ Medicaid spending by $1.8 billion over 10 years.
.


